Key Takeaways
- Skill Progression Roadmap: Mastering the integration of mental health and substance use care takes time. Expect to spend 3-6 months refining your approach to dual diagnosis treatment planning.
- Essential Tools: Familiarize yourself with the ASAM Criteria, evidence-based therapies (like CBT and MET), and secure telehealth platforms to deliver comprehensive care.
- Competency Checklist: You are ready to advance when you can confidently design a unified treatment plan that addresses both psychological distress and substance use simultaneously.
- Professional Impact: Implementing structured, culturally grounded programs—like the Wellbriety approach—enhances engagement and improves long-term outcomes in any Montana rehab setting.
What Makes Montana Rehab Treatment Trustworthy
ASAM Criteria as Your Foundation
In this section, you’ll learn why the ASAM Criteria is the backbone of trustworthy Montana rehab programs—and how to recognize when it’s being used effectively in your practice. You’ll know you’ve learned it when you can spot the key features of ASAM-based care and explain why they matter for patient safety and clinical outcomes.
Think of the ASAM Criteria as a detailed architectural blueprint guiding each person’s treatment journey. Instead of offering the same path to everyone, this approach uses six dimensions—from withdrawal risk to daily living needs—to design a care plan unique to each individual. This is especially crucial in our field, where residents face substance use disorders at rates 1.5 times the national average, and mental health distress is rising sharply.6,3
ASAM Criteria isn’t just a best practice; it’s required for all licensed facilities by the state health department. Programs using this foundation must create personalized treatment plans, often within 24 to 48 hours of admission, using input from a multidisciplinary team of professionals. Yes, this rapid turnaround is challenging, but every step forward counts toward building a safer environment for those in your care.1
| Dimension | Focus Area | Clinical Application |
|---|---|---|
| 1 | Acute Intoxication/Withdrawal | Medical management and stabilization needs |
| 2 | Biomedical Conditions | Physical health complications requiring concurrent care |
| 3 | Emotional/Behavioral Conditions | Dual diagnosis and psychiatric integration |
| 4 | Readiness to Change | Motivational enhancement strategies |
| 5 | Relapse/Continued Use Potential | Coping skills and trigger management |
| 6 | Recovery Environment | Housing, family support, and community resources |
Practice This: Create a sample treatment plan using the six ASAM dimensions. Identify what information you’d need at each step. When documenting in your electronic health record (EHR), you might use a keyboard shortcut like Ctrl + D to pull up the ASAM_Dimension_Array template. This ensures you never miss a critical domain.
Skill Checkpoint: You’re ready for the next level when you can outline how ASAM Criteria ensures care is both safe and tailored for each person without relying on a reference sheet.
- Business Application Track: Following ASAM Criteria helps clinical teams coordinate care efficiently, supports better documentation for payer reimbursement, and reduces liability.
- Personal/Clinical Use Track: Understanding these criteria gives you the confidence that the care you are providing or recommending is genuinely individualized, not one-size-fits-all.
Every step you take in mastering ASAM-based care supports a safer, more effective Montana rehab experience. Next, let’s look at why state licensing standards provide another layer of protection.
State Licensing Standards Matter
In this section, you’ll learn how state licensing standards set the baseline for safety and quality in any Montana rehab setting—and how to spot when those standards are being upheld. You’ll know you’ve learned it when you can identify what state licensing requires and why it matters for both compliance and real-world outcomes.
Picture licensing standards as the safety rails on a bridge. They keep everyone moving forward safely, no matter the weather. In our state, licensed substance use disorder programs must follow strict rules on staffing, record-keeping, individualized care planning, and facility safety. These requirements aren’t just paperwork—they’re designed to prevent harm, ensure appropriate supervision, and guarantee each person’s unique needs are addressed within set timeframes.1
“Licensing standards aren’t just administrative hurdles; they are the architectural blueprint for patient safety and clinical excellence.”
For example, regulations require treatment plans to be completed quickly after admission—within 24 to 48 hours for higher-intensity care levels. Only licensed professionals can provide certain services, and all staff must meet training standards. These steps protect individuals and make sure programs are ready for urgent needs. In addition, licensing standards allow for regular inspections and ongoing oversight, creating a culture of accountability that benefits everyone involved.1
Practice This: Review a sample facility’s licensing checklist. Note which requirements protect client safety and which support effective care planning.
Skill Checkpoint: You’re ready for the next level when you can explain to a colleague how state licensing standards support both safety and individualized care in Montana rehab settings.
- Business Application Track: Licensing compliance helps teams avoid regulatory setbacks, secures high-reimbursement payer partnerships, and supports sustainable operations.
- Personal/Clinical Use Track: Knowing your program is licensed means you can trust the environment is safe, ethical, and focused on holistic well-being.
With these foundations in place, you’re ready to explore why dual diagnosis care is especially vital for our population.
Dual Diagnosis Care in Montana Rehab Settings
Why Integrated Treatment Works Better
In this section, you’ll learn why integrated treatment—where substance use and mental health conditions are addressed together—leads to better outcomes for Montana rehab participants. You’ll know you’ve learned it when you can explain how this approach improves both recovery rates and day-to-day stability for people with co-occurring challenges.
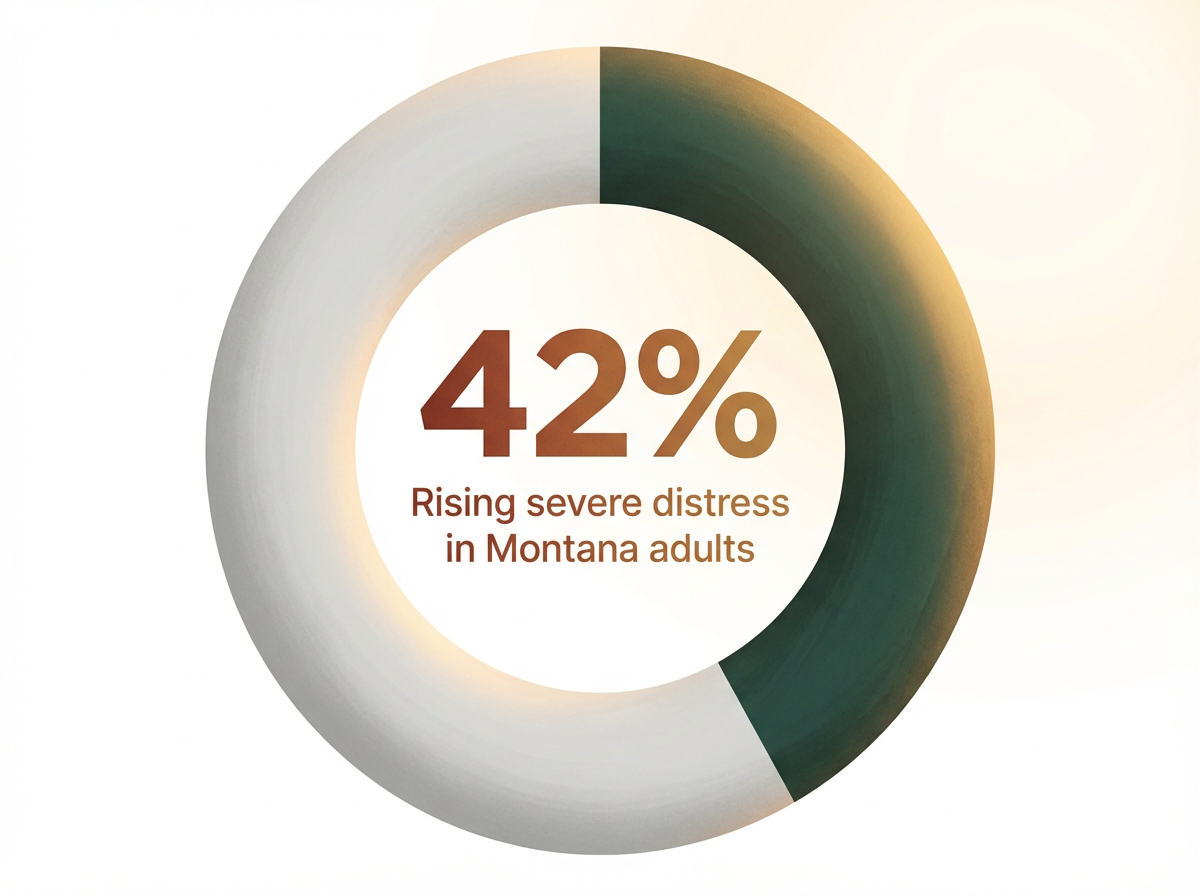
Imagine trying to fix a leaky roof and a broken furnace in the same house, but hiring two separate teams who never talk to each other. Progress stalls, and problems overlap. That’s what happens when substance use and mental health are treated separately. Integrated treatment brings both issues under one coordinated plan, with a single team working side by side. This is especially important in our region, where over 21 million U.S. adults experience both conditions, and severe psychological distress has risen by 42% statewide in the last decade.3,6
Deep Dive: The Neuroscience of Co-occurring Conditions
When treating dual diagnosis, we are often addressing overlapping neural pathways. Anxiety and depression can dysregulate the brain’s reward system, making substance use a highly reinforced coping mechanism. Integrated care simultaneously soothes the nervous system while building new, healthier neural pathways for emotional regulation.Research shows that integrated care is more effective than traditional “sequential” or “parallel” approaches, which can leave gaps and confusion for both patients and providers. People are less likely to drop out of care, and behavioral therapies adapted for both depression/anxiety and substance use have stronger results—especially when delivered by the same clinicians. You are doing great work by shifting toward this unified model.8
Practice This: Outline a weekly schedule for a hypothetical client in a Montana rehab setting. Make sure both mental health therapy and substance use counseling are included together, not in isolation.
Skill Checkpoint: You’re ready for the next level when you can describe how one treatment plan—managed by a single team—prevents people from falling through the cracks.
- Business Application Track: Integrated care supports operational efficiency and reduces staff burnout by streamlining communication across departments.
- Personal/Clinical Use Track: Integrated treatment means your clients won’t have to repeat their story or juggle conflicting advice—they get support for their whole self, every step of the way.
Evidence-Based Therapies for Co-Occurring Conditions
In this section, you’ll discover which evidence-based therapies help people with co-occurring mental health and substance use conditions thrive in a Montana rehab setting. You’ll know you’ve learned it when you can explain how these therapies work together to address both sides of dual diagnosis—and why they’re considered best practice.
Think of evidence-based therapies as sturdy tools in a craftsman’s toolbox, each designed for a specific job. Cognitive Behavioral Therapy (CBT) is a prime example: it’s been shown to help 58% of participants achieve better outcomes than other approaches, especially when anxiety or depression is part of the picture. In Montana rehab programs, CBT can be adapted to help clients recognize thoughts that fuel both substance use and overwhelming emotions, making it easier to break out of self-defeating cycles.7
Motivational Enhancement Therapy (MET) is another key tool. This approach helps clients find their own reasons for change, boosting engagement and retention—important in a state where sticking with treatment can be challenging due to distance or isolation. Therapies like Dialectical Behavioral Therapy (DBT) and trauma-informed care are also vital, as nearly half of people with substance use disorders experience significant trauma symptoms.4,7
// Sample Dual Diagnosis Treatment Protocol
Phase 1: Stabilization & Assessment (ASAM Dimensions 1-3)
Phase 2: Integrated CBT + MET Sessions (Addressing Triggers & Motivation)
Phase 3: Trauma-Informed Processing (DBT Skills & Emotional Regulation)
Phase 4: Maintenance & Recovery Housing Integration
Practice This: Pick a therapy—like CBT or MET—and map out a session that addresses both substance use and a common mental health challenge, such as depression or anxiety.
Skill Checkpoint: You’re ready for the next level when you can describe how adapting therapy for dual diagnosis creates a more supportive recovery environment.
- Business Application Track: Using evidence-based therapies helps teams measure progress, train staff consistently, and demonstrate effectiveness to stakeholders and referral partners.
- Personal/Clinical Use Track: Knowing your Montana rehab uses proven therapies means you can trust the treatment is grounded in real results, not guesswork.
Overcoming Montana’s Geographic Barriers
Virtual Programs Expand Access Statewide
In this section, you’ll learn how virtual programs are transforming access to Montana rehab for people across the state—no matter how rural or remote their community. You’ll know you’ve learned it when you can explain why virtual care breaks down traditional barriers and how to assess if this model supports both clinical outcomes and participant engagement.
Picture our geography as a patchwork of wide-open spaces and distant communities, where a single trip to a clinic might take hours. Virtual programs act like bridges, letting individuals connect with care teams, therapy groups, and resources without ever leaving home. For those in “frontier” counties—80% of the state’s land area—this isn’t just convenient, it’s essential.2
Recent studies show that virtual Intensive Outpatient Programs (IOPs) aren’t just a backup plan; they can be highly effective. Nearly 45% of participants in telehealth IOPs successfully completed treatment or stepped down to a lower level of care, and 80% finished at least 30 days of continuous participation. Virtual options also ease workforce shortages and allow teams to provide specialized dual diagnosis support statewide, overcoming the limits of local staffing.5
Practice This: Map out how a client in a remote town could access group therapy, individual counseling, and medication management using virtual tools. Identify what technology and local support would be needed.
Skill Checkpoint: You’re ready for the next level when you can outline how virtual Montana rehab programs make high-quality, integrated care possible—regardless of someone’s zip code.
- Business Application Track: Virtual expansion widens your reach, smooths scheduling, and supports continuity of care for hard-to-serve populations.
- Personal/Clinical Use Track: Virtual programs mean you can facilitate help from anywhere—allowing clients to balance recovery and their responsibilities at home.
In-Person Care in Montana Communities
In this section, you’ll learn why in-person care is still a trusted and essential option for Montana rehab participants—local residents and visitors alike. You’ll know you’ve learned it when you can explain how face-to-face services create unique opportunities for healing, community, and accountability, even in the face of geographic challenges.
Think of in-person rehab as a sturdy gathering place in the middle of a vast landscape—a hub where people come together, find support, and build routines that strengthen recovery. While virtual care has expanded reach, some individuals need the structure and hands-on support of in-person programs. This is especially true for people facing complex mental health or substance use issues, or those who benefit from the consistency of daily routines and group connection.
Research shows that residential and structured in-person programs achieve a 65% completion rate—significantly higher than standard outpatient settings at 52%—highlighting the value of immersive, community-based treatment. On-site care also makes it easier to access medical support, peer recovery groups, and trauma-informed therapies that require a safe, controlled environment. In many communities, these programs become a lifeline, offering a sense of belonging and hope when distance or isolation might feel overwhelming.10
Practice This: Walk through a day in a Montana rehab facility. Identify moments where face-to-face interaction, shared meals, or group therapy add value that’s hard to replicate virtually.
Skill Checkpoint: You’re ready for the next level when you can outline why someone might choose in-person care—even if virtual options are available.
- Business Application Track: In-person programs foster local partnerships, create jobs, and anchor recovery resources in the community.
- Personal/Clinical Use Track: Attending in person helps clients rebuild routines, find new friends, and experience the encouragement that comes from real-world connection.

Choosing the Right Level of Care
When you’re ready to guide a client to the next step in their recovery journey, choosing the right level of care becomes one of your most important clinical decisions. You know their patterns, their triggers, and what hasn’t worked before—now it’s about matching that clinical knowledge with the structure and support that fits where they are today.
Partial hospitalization programs provide intensive therapeutic support when individuals need significant structure but can maintain stability outside 24-hour medical supervision. The question isn’t whether you understand what partial hospitalization programs offer—it’s whether this level matches the client’s current readiness and circumstances. Are they transitioning from residential care and need continued intensive support? Do they have co-occurring mental health concerns that require comprehensive daily attention? Can they maintain accountability with evening and weekend autonomy? These questions help determine if partial hospitalization programs align with their recovery needs right now.
Intensive outpatient programs create space for meaningful therapeutic engagement while clients navigate work, family, and daily responsibilities. You’re not looking for basic definitions of intensive outpatient programs—you’re assessing whether they’ve built enough recovery skills to manage increased independence. Can they implement coping strategies between sessions? Do they have some support system stability? Are they ready to practice recovery skills in real-world situations while still receiving structured guidance? Intensive outpatient programs work when they are prepared for this balance.
Virtual partial hospitalization programs and virtual intensive outpatient programs deliver the same clinical rigor through secure online platforms, removing geographic and logistical barriers. If you’re working with professionals managing treatment around career commitments, or individuals in a rural area without local access to specialized dual diagnosis care, virtual partial hospitalization programs and virtual intensive outpatient programs provide full therapeutic support without compromising their other responsibilities. At facilities like Healing Rock Recovery, virtual programs integrate the same evidence-based therapies, medication-assisted treatment coordination, and trauma-informed approaches as in-person care, with scheduling flexibility designed specifically for adults balancing professional lives.
Assessing the right level of care means honest evaluation of several factors: severity and patterns of substance use, co-occurring mental health conditions, stability of the current environment, what has been learned from previous treatment experiences, and the demands of daily life. You’re not sorting people into categories—you’re identifying which structure provides enough support without creating dependency on more intensity than serves their growth.
Levels of care adapt as progress is made. A client might begin with partial hospitalization programs and transition to intensive outpatient programs as they demonstrate readiness for increased autonomy. An integrated approach to dual diagnosis treatment in a Montana rehab means your care team adjusts programming based on evolving needs, not arbitrary timelines. What matters is choosing a starting point that provides the foundation needed for sustainable healing while respecting the life being built in recovery.
Frequently Asked Questions
How long should you stay in treatment for lasting results?
For lasting results, a minimum treatment duration of 90 days is widely supported by research on substance use disorder recovery. Stays shorter than this are linked to higher relapse rates and lower completion, while longer engagement gives your brain and body the time they need to heal and build new habits. Montana rehab programs often offer flexible options, but the most positive outcomes come from steady participation—whether that’s in residential, outpatient, or virtual formats. Remember, progress is not always linear, and it’s normal to need more support at different points in your journey. Every day in treatment strengthens your foundation for long-term recovery.4
What happens if you need to switch between virtual and in-person care?
Switching between virtual and in-person care in a Montana rehab setting is a flexible, supportive process designed to fit your changing needs. If your situation shifts—maybe due to travel, a new job, or a health concern—your treatment team will help you transition smoothly. Most programs coordinate to keep your therapy schedule, group participation, and medication management as consistent as possible, so you don’t lose momentum. Research shows that virtual Intensive Outpatient Programs (IOPs) in Montana have high engagement, with 80% of participants completing at least 30 days of care, making transitions between formats both common and successful. You’re never locked into just one type of care; the goal is to keep you connected, supported, and on track no matter where you are. 5
Can you work or attend school while participating in treatment programs?
Yes, you can often work or attend school while participating in Montana rehab programs—especially with flexible options like Intensive Outpatient Programs (IOP) or Partial Hospitalization Programs (PHP). These formats are designed to fit around your responsibilities, offering sessions during evenings or outside standard work hours. Virtual IOPs, in particular, allow you to access therapy from home, making it easier to balance treatment with job or class schedules. If you need a higher level of care, your treatment team can help coordinate school or work accommodations. Remember, each small step forward—balancing recovery and daily life—is a real achievement.5
How do treatment teams address both anxiety and substance use together?
Treatment teams in Montana rehab settings address anxiety and substance use together by using integrated, evidence-based approaches like Cognitive Behavioral Therapy (CBT). Instead of treating anxiety and substance use separately, clinicians work as a unified team to create a single, coordinated plan that targets both issues at once. For example, adapted CBT helps you recognize how anxious thoughts can fuel cravings, while also building healthy coping skills for both anxiety and substance triggers. Research shows that this kind of integrated care leads to stronger, more lasting progress for people facing both challenges. Small steps matter—every session builds resilience on both fronts.8
What makes treatment completion rates higher in some settings?
Higher completion rates in some Montana rehab settings come down to the right match between environment, support, and structure. Residential programs, for example, see about 65% of participants finish treatment—much higher than the 52% seen in outpatient care. Why? Immersive settings offer fewer distractions, a sense of community, and daily routines that keep people engaged. Consistent support from staff and peers can help you stay motivated, especially when recovery feels tough. Remember, every day you stick with it is a step forward. Programs that adapt to your needs—like offering both in-person and virtual care—also boost the odds you’ll complete treatment.10
How do you know if virtual treatment will work as well as in-person care?
Wondering if virtual treatment can be as effective as in-person care? Recent research shows virtual Intensive Outpatient Programs (IOPs) in Montana rehab settings have a 44% successful response rate, with 80% of participants completing at least 30 days—matching or even surpassing many in-person engagement rates. The right fit depends on your needs: virtual care offers flexibility and removes travel barriers, especially for those in remote areas, while in-person care may provide more structure and face-to-face support. If you can stay engaged and access the technology required, virtual treatment can absolutely support strong recovery outcomes.5

Finding Your Path to Healing in Montana
Once you’ve identified the right level of care for your clients’ needs, the next step is finding a provider whose approach truly aligns with their recovery goals. Taking the step toward recovery is deeply personal, and finding the right support can feel overwhelming. They deserve a substance use treatment environment that sees them as a whole person—not just a diagnosis. A Montana rehab landscape offers something distinctive for healing: wide-open spaces that create natural distance from triggers, a pace that allows genuine reflection, and providers who integrate evidence-based care with approaches you won’t find everywhere—like the Wellbriety program, which brings Indigenous healing practices into modern substance use treatment frameworks.
When you’re exploring substance use treatment options for your referrals, consider what will actually support their success. Does the provider offer integrated dual diagnosis expertise, addressing both substance use and mental health challenges simultaneously rather than treating them separately? If faith or cultural background matters to their healing, does the program honor those elements as clinical assets rather than afterthoughts? For professionals balancing recovery with work responsibilities, can the program offer flexible scheduling or virtual options that protect privacy while delivering the same therapeutic intensity? These aren’t just preferences—they’re essential factors that determine whether treatment fits real life.
The right path forward combines evidence-based substance use treatment with compassionate support tailored to specific needs. Look for providers who demonstrate cultural competency, offer trauma-informed approaches across all services, and can point to concrete resources—whether that’s medically assisted treatment protocols, creative therapies that address healing beyond talk therapy, or recovery housing that extends support beyond clinical hours. The Montana rehab community understands that lasting change happens when clinical excellence meets genuine understanding of who the individual is and what they are facing. You don’t have to navigate this alone—the right provider will walk alongside you and your clients every step of the way.
References
- Montana Department of Public Health and Human Services Rules for Substance Use Disorder Facilities. https://dphhs.mt.gov/assets/oig/Rules_for_Substance_use_Disorder_Facility.pdf
- National Disability Navigator: Substance Abuse Challenges in Rural Areas. https://nationaldisabilitynavigator.org/2014/02/25/overcoming-substance-abuse-challenges-in-rural-areas-part-i/
- Montana BRFSS: Changes in Severe Psychological Distress Among Montana Adults. https://dphhs.mt.gov/assets/publichealth/BRFSS/ChangesInSeverPsyDistressAmongMTAdults2012-2021.pdf
- Evidence-Based Practices for Substance Use Disorders (NIH). https://pmc.ncbi.nlm.nih.gov/articles/PMC3678283/
- Patient Engagement in Providing Telehealth SUD IOP Treatment. https://pmc.ncbi.nlm.nih.gov/articles/PMC11675410/
- Substance Use & Mental Health Statistics. https://boards.bsd.dli.mt.gov/_docs/med/SUD-MHD-Stats.pdf
- Efficacy of Cognitive Behavioral Therapy: Meta-Analysis Review. https://pmc.ncbi.nlm.nih.gov/articles/PMC3584580/
- Integrating Treatment for Co-Occurring Mental Health Conditions. https://pmc.ncbi.nlm.nih.gov/articles/PMC6799972/
- Barriers for Implementing Hub and Spoke Model in Rural Areas. https://pmc.ncbi.nlm.nih.gov/articles/PMC8411614/
- Residential and Outpatient Treatment Completion. https://pubmed.ncbi.nlm.nih.gov/26925821/






