Key Takeaways: Your Path Forward
- Assessment Scoring: If you find that treating one condition causes the other to flare up, you likely require integrated care rather than sequential treatment.
- Success Factors: Long-term remission rates jump to over 62% when mental health and substance use are treated simultaneously by a coordinated team10.
- Immediate Action: Use the 30-day plan in Section 4 to schedule a dual-licensed evaluation, prioritizing programs that offer “integrated” rather than “parallel” services.
What Understanding Dual Diagnosis Reveals
Understanding dual diagnosis illuminates the intricate relationship between psychiatric disorders and substance use disorders—a connection that affects millions of people seeking recovery. When you grasp this concept, you begin to see why traditional treatment approaches often fall short for those experiencing both challenges simultaneously.
Dual diagnosis shows that psychiatric disorders and chemical dependencies frequently develop together, each influencing and intensifying the other. Research demonstrates that approximately 50% of individuals with severe psychiatric conditions also experience problematic drug or alcohol use at some point in their lives.
Common pairings you might encounter include:
- Depression alongside alcohol use disorder.
- PTSD combined with opioid addiction.
- Anxiety disorders coupled with sedative misuse.
Recognizing these patterns helps explain why you might turn to substances as a way to manage untreated anxiety, depression, or trauma symptoms—a pattern known as self-medication. What understanding dual diagnosis truly demonstrates is that these intertwined conditions require integrated treatment rather than separate, disconnected approaches. When your treatment addresses only addiction without considering underlying psychiatric concerns, or vice versa, the likelihood of lasting recovery significantly decreases.
Recognizing dual disorders also highlights the importance of comprehensive assessment. What may appear as symptoms of chemical misuse in your case could actually stem from an underlying psychiatric condition, or symptoms that seem like mental illness might result from drug- or alcohol-related changes in your brain chemistry. This complexity requires clinical expertise to properly identify and address both concerns you’re facing.
“Embracing this perspective means recognizing that healing is possible when treatment acknowledges you as a complete person, not just individual diagnoses.”
With this foundation established, you can better appreciate the tangible outcomes that integrated dual diagnosis treatment delivers.
The Hidden Connection Between Two Struggles
When you start looking at dual diagnosis, it’s easy to miss how deeply mental health and substance use issues can influence one another. Sometimes, what seems like a single challenge is actually two struggles feeding off each other beneath the surface. Many people living with anxiety or depression may use substances to cope, while others find that substance use sparks new mental health symptoms.
This cycle makes co-occurring disorders more common than you might expect—about one in three adults with a mental health condition also faces substance use challenges6. Recognizing this hidden connection is a powerful step. It can help you break free from shame and realize that integrated care, not blame or isolation, is the path toward healing.
How Mental Health and Substance Use Intertwine
Mental health and substance use can become tangled together in ways that are hard to see at first. For example, someone living with depression might turn to alcohol, hoping for relief, while ongoing substance use may trigger or worsen symptoms of anxiety or mood disorders.
Genetics, trauma, and stress all play a part in this relationship:
- Genetics: Research shows that up to 60% of a person’s risk for developing a substance use disorder may be linked to their genes7.
- Trauma: Early life stress raises the chances of developing both mental health and substance use challenges6.
This complex connection is why professionals talk about co-occurring disorders or integrated treatment: because both issues often need attention at the same time for real progress. When you’re focused on understanding dual diagnosis, you begin to see how these struggles often reinforce each other, making compassion and teamwork essential in your recovery journey.
Why 35% of Adults Face Both Conditions
You might wonder why as many as 35% of adults end up living with both a mental health condition and a substance use disorder. This overlap isn’t just a number—it’s shaped by real-life experiences like trauma, genetics, and self-medicating tough emotions.
Research points out that more than 30% of adults with substance use disorders have experienced childhood trauma, which can make both types of challenges more likely to appear together6. When coping skills or support systems fall short, people often try to manage mental health symptoms through substances, leading to co-occurring disorders. Recognizing these root causes helps you approach understanding dual diagnosis with more self-compassion and less blame.
Self-Assessment: Recognizing Co-Occurring Signs
Here’s a quick self-assessment tool to help you recognize if both mental health and substance use patterns might be showing up in your life. Grab a notepad or open an app—reflect on symptoms like ongoing sadness, anxiety, or mood swings along with changes in your use of alcohol or other substances.
Notice if one issue seems to trigger the other, or if both challenges are making daily life harder. This process is not about judgment—it’s about understanding dual diagnosis and gaining clarity. If you spot patterns that match common co-occurring disorders, that’s a sign to explore integrated support.
Diagnostic Questions for Your Situation
To help you get clearer about whether co-occurring challenges are impacting your life, try answering these diagnostic questions. You can mentally check Yes or No for each:
- In the past six months, have you noticed frequent sadness, anxiety, or mood swings alongside increased use of alcohol or other substances?
- Do you find that using substances makes your mental health symptoms worse?
- Do emotional struggles push you to use more substances than intended?
- Are there times when managing one issue seems to make the other harder?
If you answered ‘yes’ to any of these, you may be experiencing overlapping concerns. These questions are a starting point for understanding dual diagnosis and can guide you in seeking more integrated support.
Understanding Dual Diagnosis in Your Life
Understanding dual diagnosis in your life is about recognizing how overlapping mental health and substance use patterns may be shaping your daily experience. You might notice that addressing one concern without the other leaves you feeling stuck, or that emotions and substance use seem to fuel each other over time.
Integrated care, which treats both mental health and substance use concerns together, is proven to offer better outcomes than separate approaches4. Remember, identifying co-occurring disorders or substance use triggers is never a sign of weakness—it’s a step toward greater self-awareness.
Why Understanding Dual Diagnosis Changes Outcomes
When you grasp the interconnected nature of dual disorders, you gain access to treatment that addresses the complete picture of your psychological wellbeing. This comprehensive approach fundamentally transforms recovery outcomes because it recognizes that treating only one condition while ignoring the other creates an incomplete path forward.
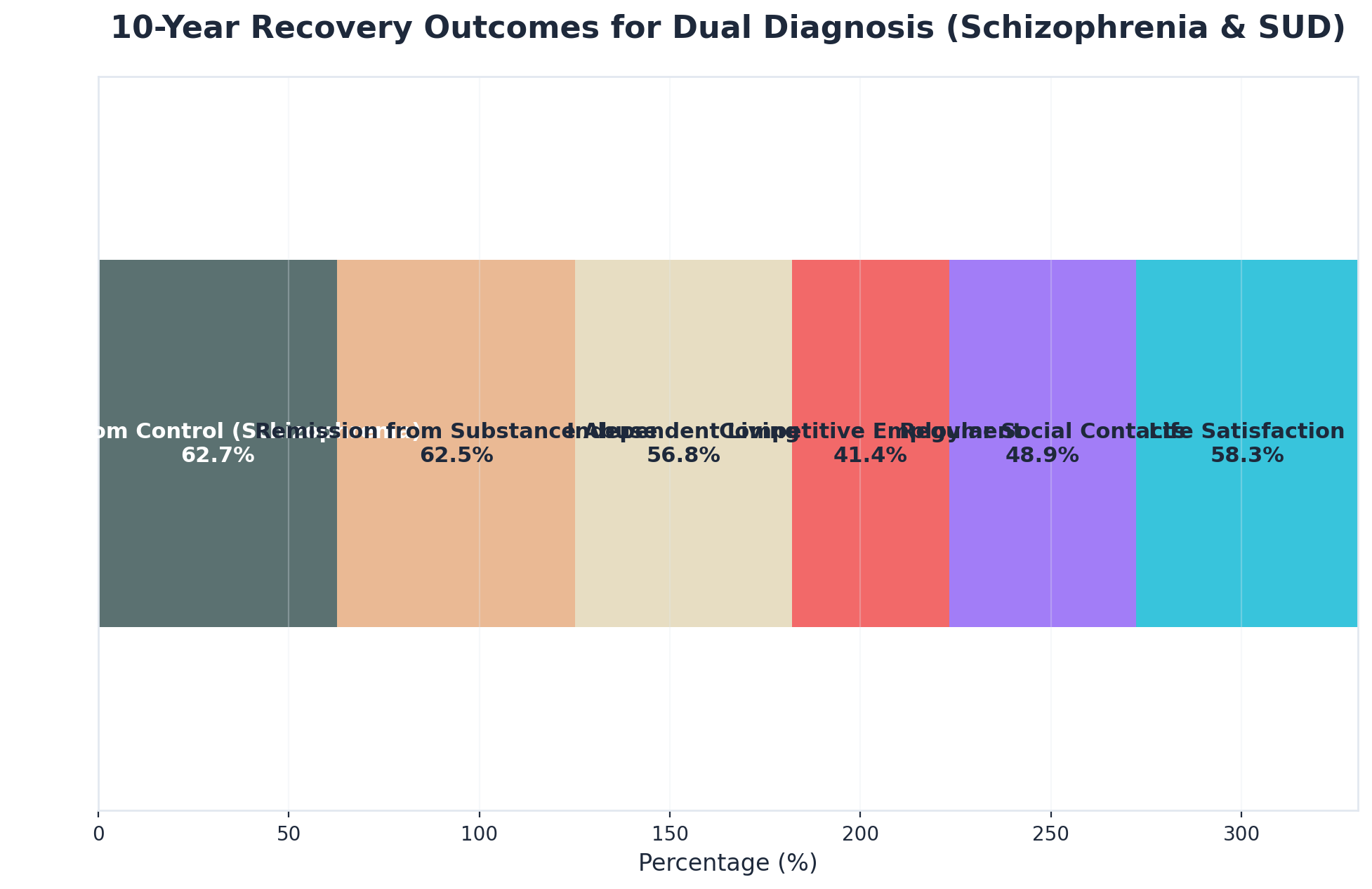
Research consistently demonstrates that integrated treatment for overlapping psychiatric and addiction disorders produces significantly better results than addressing emotional challenges separately from dependency issues. When you receive care that tackles both issues simultaneously, you’re more likely to maintain long-term recovery, experience fewer relapses, and develop stronger coping mechanisms that support your overall wellbeing.
Grasping the relationship between these conditions also helps you make sense of patterns that may have felt confusing or overwhelming. You might have noticed that your anxiety intensified your drinking or drug use, or that using alcohol or drugs temporarily relieved depression symptoms before making them worse. Recognizing these connections allows your treatment team to develop strategies that interrupt these cycles rather than inadvertently reinforcing them.
The dual diagnosis framework changes outcomes because it eliminates the frustrating experience of bouncing between different providers who only address part of your situation. Instead of receiving psychiatric care in one setting and addiction treatment in another, you benefit from coordinated services where professionals communicate and collaborate on your behalf.
Perhaps most importantly, understanding dual diagnosis empowers you to become an active participant in your healing. When you comprehend how your disorders influence each other, you can recognize warning signs earlier, communicate more effectively with providers, and make informed decisions that support your sustained recovery and psychological wellness.
The Cost of Fragmented Treatment Approaches
Fragmented treatment—where mental health and substance use disorders are addressed separately—can leave you feeling like you’re caught in a tug-of-war. When programs don’t communicate, important information gets lost, and your care plan may feel incomplete.
Research shows that only 9.1% of people with both conditions receive care for both, while more than half (52.5%) get no treatment at all6. If you’re trying to manage co-occurring disorders with disconnected support, it’s easy to lose hope or feel stuck. Prioritizing integrated care means you’re not forced to choose which struggle to address first.
Why 52.5% Receive No Treatment at All
It’s heartbreaking to see that 52.5% of people with co-occurring mental health and substance use challenges receive no treatment at all6. This gap often happens because services are split up—mental health clinics and substance use programs may not work together, leaving you feeling like you have to choose which struggle matters more.
Insurance rules, long waitlists, and a shortage of integrated programs can also make it tough to get the right help. If you’re navigating co-occurring disorders, you might be turned away or told to get one issue “under control” before addressing the other. This scattered approach makes accessing care for understanding dual diagnosis frustrating and discouraging for many.
The Double Stigma That Prevents Healing
Facing both mental health and substance use challenges can feel like carrying two invisible weights—and stigma is a big reason why many people don’t reach out for help. This “double stigma” happens when you experience judgment or misunderstanding about both struggles at once, leading to extra shame and isolation.
“Studies show that these negative attitudes from society, family, or even some care providers can stop you from seeking the support you truly need.”5
Breaking free from the double stigma begins with understanding dual diagnosis and recognizing that both mental health and substance use conditions deserve empathy and integrated care. When you embrace co-occurring disorders as a real medical issue, not a character flaw, you open the door to healing and connection.
Decision Framework: Integrated vs Sequential Care
When you’re deciding between integrated and sequential care for co-occurring disorders, a clear framework can help you choose what fits best. Start by asking: Are your mental health and substance use symptoms connected and making each other worse?
| Feature | Integrated Care | Sequential Care |
|---|---|---|
| Approach | Treats both conditions simultaneously. | Treats one condition, then the other. |
| Team Structure | One coordinated team. | Separate providers/clinics. |
| Outcome | Lower relapse rates, higher satisfaction4. | Higher risk of relapse during transition. |
If you’ve tried one-at-a-time approaches and felt frustrated or stuck, you’re not alone. Integrated treatment is recommended for most people with co-occurring disorders and is especially important when symptoms overlap daily or have not improved with separate care.
Clear Criteria for Effective Treatment Models
To help you spot truly effective care for co-occurring mental health and substance use conditions, use this criteria checklist:
- Does the program offer integrated treatment where both issues are addressed at the same time by a single, coordinated team?
- Are counseling, medication support, and peer recovery groups available within one setting?
- Is trauma-informed care included, recognizing how past experiences shape dual challenges?
- Are you involved in shaping your treatment plan, with regular check-ins and adjustments?
Research confirms that programs meeting these standards lead to better results and fewer setbacks for those focused on understanding dual diagnosis4. This approach is ideal for anyone facing overlapping symptoms or who has tried treating one issue at a time without success.
Understanding Dual Diagnosis Through Evidence
When you want confidence in your treatment choice, looking at the science behind understanding dual diagnosis can make a huge difference. Research shows that people who receive integrated care—where mental health and substance use concerns are addressed together—have fewer relapses and better long-term outcomes than those who try to tackle each issue separately4.
For example, ten-year studies reveal that over 62% of individuals with co-occurring disorders reach remission from substance abuse, and nearly 58% report real life satisfaction after sustained integrated support10. These results highlight why co-occurring disorders need an approach that treats both sides at once.
Implementation Pathways for Your Recovery
Now that you understand why integrated treatment works, the next step is determining which pathway fits your specific situation. The right level of care depends on several factors: the severity of your symptoms, your living environment, previous treatment history, daily responsibilities, and—realistically—your insurance coverage and financial resources.

Consider Residential Treatment if you’re experiencing severe symptoms, have safety concerns, or haven’t found success with outpatient approaches. Residential treatment programs for concurrent psychiatric and addiction conditions provide the most comprehensive level of care, offering 24/7 support in a structured environment. These programs typically last 30 to 90 days and allow for complete focus on recovery while medical professionals address both your emotional well-being and chemical dependency simultaneously.
Partial Hospitalization Programs (PHP) offer intensive integrated care while allowing a return home each evening. You’ll participate in therapy and medical monitoring for several hours daily, typically five to seven days per week. This pathway bridges the gap between residential care and traditional outpatient services, providing substantial support while maintaining some connection to daily life.
Intensive Outpatient Programs (IOP) work well if you have a stable living situation, supportive relationships, and can manage symptoms between sessions. These programs deliver coordinated treatment for overlapping psychological and addiction challenges through scheduled sessions several times weekly, usually totaling 9-12 hours of treatment per week. This flexibility enables maintaining work or family responsibilities while receiving professional care.
Standard Outpatient Care for dual diagnosis conditions involves weekly or bi-weekly appointments with behavioral health professionals and addiction specialists who coordinate treatment. This pathway suits those with stable living situations and milder symptoms, or serves as ongoing maintenance after completing more intensive programs.
Matching Treatment Intensity to Your Needs
To help you match treatment intensity to your needs, start with this decision checklist:
- Are your mental health and substance use symptoms causing daily disruptions?
- Do you need a structured environment with frequent support, or can you manage with more flexibility?
- Is trauma or stress making your symptoms worse?
Understanding dual diagnosis means you have options, and the best fit depends on your current situation. For some, a structured approach like partial hospitalization works best when symptoms feel overwhelming. For others, intensive outpatient care offers flexibility for those balancing recovery with work, school, or family.
Partial Hospitalization for Dual Conditions
Partial hospitalization programs (PHPs) give you a highly structured, daytime environment while allowing you to return home in the evenings. This approach works best when your mental health and substance use symptoms feel too overwhelming for outpatient care, but you don’t need 24/7 supervision.
In a PHP, you’ll usually spend 20–30 hours a week on-site, with a team that addresses both co-occurring disorders at once—using therapy, medication support, and peer recovery groups. Research confirms that this integrated care model leads to more progress and fewer setbacks compared to treating each challenge separately4.
Intensive Outpatient Options for Flexibility
Intensive outpatient programs (IOPs) give you the chance to keep making progress toward recovery while staying connected to your daily responsibilities. This solution fits when you want structured treatment for co-occurring disorders but also need the flexibility to continue working, caring for family, or keeping up with school.
In an IOP, you typically attend therapy and group sessions three to five times per week, usually for 9–15 hours total, all while returning home each day. This approach is ideal for anyone whose symptoms are stable enough to not need full-time supervision, but who still benefits from regular, integrated support addressing both mental health and substance use.
Resource Planning for Sustainable Recovery
Planning your resources for sustainable recovery helps you turn understanding dual diagnosis into action that lasts. Start by building a checklist of what you’ll need: integrated therapy options, support groups, medication management, and flexible scheduling to fit your life.
Most people succeed when they combine counseling, peer support, and trauma-informed care—these resources work together to address both mental health and substance use at once4. Virtual treatment and evening programs can be especially helpful if you’re balancing work or family, making real-world recovery more accessible than ever6.
Therapy Modalities That Address Both Issues
When you’re planning for lasting recovery, choosing therapy modalities that address both mental health and substance use together is key.
- Cognitive Behavioral Therapy (CBT): Helps you change negative thinking patterns.
- Trauma-Informed Care: Focuses on how past experiences shape current challenges.
- Motivational Interviewing: Supports you in building confidence and motivation for change.
- Peer Support Groups: Offer connection and understanding from others walking a similar path.
These therapy options work best when integrated—meaning you address co-occurring disorders in the same setting with a coordinated team. Research shows that combining these modalities as part of integrated care leads to better results and fewer setbacks for people focused on understanding dual diagnosis4.
Understanding Dual Diagnosis Recovery Timelines
When you’re building a plan for understanding dual diagnosis, it helps to know what recovery timelines often look like. Progress is rarely a straight line—integrated treatment for co-occurring disorders typically unfolds over months and sometimes years, depending on your unique story and the resources you have.
Long-term studies show that more than 62% of people with both mental health and substance use challenges reach remission from substance abuse after ten years of sustained, integrated care10. This shows that steady, ongoing support for co-occurring disorders leads to real progress and greater quality of life.
Your Next 30 Days: An Action Plan for Understanding Dual Diagnosis
You might be reading this plan and feeling uncertain—maybe even overwhelmed. That’s completely normal. You don’t have to feel 100% ready to take action, and it’s okay if part of you is still hesitant. Recovery doesn’t require certainty; it just requires one small step forward. This practical action plan breaks down your journey into manageable steps that build momentum and create lasting change.

- Week 1: Research and Reach Out
Begin by researching treatment options that align with your needs. Look into inpatient programs, outpatient services, and support groups in your area. Make at least three phone calls to treatment centers to ask questions about their approaches and availability. If making three calls feels overwhelming, start with just one—that single call is still meaningful progress. Schedule a medical evaluation to assess your current health status. - Week 2: Build Your Support Network
Identify trusted friends or family members who can support your recovery journey. Have honest conversations about your plans and the kind of help you’ll need. When researching treatment options, specifically ask about providers experienced with dual diagnosis treatment—finding professionals who understand the connection between mental health and addiction is crucial for comprehensive care. - Week 3: Create Structure and Stability
Develop a daily routine that supports your recovery goals. This includes regular sleep schedules, meal planning, and activities that promote physical and mental wellness. Remove substances and triggers from your living environment. If you’re employed, consider speaking with HR about any accommodations you might need during treatment. - Week 4: Commit and Begin
Finalize your treatment plan and set a start date. Remember that this plan can be adapted to your specific dual diagnosis needs—whether that means coordinating mental health treatment alongside addiction services or finding integrated care programs. Arrange practical matters like childcare, time off work, or transportation.
Week 1-2: Assessment and Connection Steps
Week 1 and 2 are all about laying the groundwork for your recovery by focusing on assessment and making early connections. Start with a simple checklist: schedule your first meeting with a team that understands co-occurring disorders, gather your health history, and reflect on patterns in both mental health and substance use.
Building a clear picture of your background gives your care team the tools to personalize your plan. At the same time, reach out to support groups or peer mentors who have experience with dual diagnosis recovery. Research shows that people who use integrated, trauma-informed care are more likely to see real progress with understanding dual diagnosis than those who try to tackle issues separately4.
Gathering Your Health History Information
Gathering your health history is a powerful first step toward understanding dual diagnosis and getting care that truly fits you. Start by jotting down any past diagnoses, current symptoms, and your experiences with mental health and substance use. Include details like when challenges began, any past treatments, medications, and how life events or stressors may have played a role in your journey.
If you’ve noticed patterns—like certain triggers that make symptoms worse or times when one issue seems to affect the other—write those down too. Sharing this information helps your care team spot co-occurring disorders and tailor their approach.
Understanding Dual Diagnosis Program Options
Choosing the right program is a big part of understanding dual diagnosis and setting yourself up for real progress. As you explore your options, look for programs that offer integrated care—where mental health and substance use are treated together by the same team.
This approach includes therapies like Cognitive Behavioral Therapy, trauma-informed support, and peer groups all in one setting, so you don’t have to bounce between providers. Virtual and evening programs are now available too, giving you more flexibility if you’re balancing work or family6.
Week 3-4: Beginning Your Integrated Journey
In weeks 3 and 4, you’ll move from preparation to real participation in your integrated care journey. Start by showing up for your first sessions—whether in person or virtually—and sharing the health history and goals you’ve outlined. These first weeks are about settling into a routine and getting comfortable with your care team, who will help you address both mental health and substance use challenges together.
This is where understanding dual diagnosis shifts from theory to daily practice, and you’ll notice how co-occurring disorders are supported with both therapy and peer connection. Research confirms that getting integrated, trauma-informed support during this early stage leads to better outcomes and fewer setbacks than trying to address each challenge separately4.
What to Expect in Your First Sessions
Your first sessions in integrated care for co-occurring disorders are all about building trust and easing into a new routine. You’ll meet your care team—often including a therapist, a medical provider, and a peer support specialist—who will listen to your story and review your health history together.
Expect questions about your current symptoms, recent stressors, and any goals you hope to achieve. Most programs start with gentle introductions to group therapy or peer support, so you don’t feel alone in your journey. You’ll also talk through which therapy styles, like Cognitive Behavioral Therapy or trauma-informed care, feel most comfortable for you.
Building Your Support Network Early
Building your support network early is a powerful way to keep momentum in your recovery with understanding dual diagnosis. Start by reaching out to at least one peer mentor, support group, or trusted friend who understands the challenges of co-occurring disorders. Early connection helps you feel less alone and gives you encouragement during tough days.
Consider joining a peer-led group focused on integrated recovery or asking your care team about virtual communities if in-person meetings are tough to attend. Research shows that people with strong support systems and regular check-ins are more likely to stick with their care plan and see better results for both mental health and substance use challenges4.
Frequently Asked Questions
When you’re searching for support during one of life’s most challenging moments, you likely have questions about what to expect from integrated treatment for dual diagnosis. Understanding the process can help you feel more confident about taking this important step toward healing.
How does dual diagnosis treatment differ from standard addiction treatment?
Dual diagnosis treatment addresses both your mental health condition and substance use disorder simultaneously through integrated care. Rather than treating these conditions separately, your treatment team coordinates psychiatric care and addiction recovery in a unified approach, recognizing how these conditions influence each other and require specialized, concurrent treatment.
How long does residential dual diagnosis treatment typically last?
The duration of residential care varies based on individual needs and treatment goals. Some programs last 30 days, while others extend to 60, 90 days, or longer. Your treatment team will work with you in determining the appropriate length of stay based on your progress and recovery needs.
Will I continue taking psychiatric medications during treatment?
Yes, medication management for mental health conditions is an essential component of dual diagnosis treatment. Your psychiatric team will review your current medications, make any necessary adjustments, and monitor your response throughout your stay. Some medications may be modified as you progress through treatment, always under careful medical supervision.
What happens if my psychiatric symptoms worsen during treatment?
Your clinical team continuously monitors your mental health status and can quickly adjust your treatment plan if symptoms intensify. This may include medication adjustments, increased therapy sessions, or additional psychiatric support. The residential setting provides the safety and resources needed to address symptom changes promptly.
Can I bring personal items to the treatment facility?
Most facilities allow you the opportunity to bring essential personal items like clothing, toiletries, and some comfort items. However, restrictions typically apply to electronics, certain medications, and items that could compromise safety. Your admissions coordinator will provide a detailed list of what you can bring.
What happens after I complete the program?
Successful recovery extends beyond your residential stay. Your treatment team will develop a comprehensive aftercare plan that may include outpatient therapy, support groups, medication management, and ongoing community resources supporting your continued wellness.
How do I know if I need integrated treatment for understanding dual diagnosis or if I can address one condition at a time?
You might need integrated treatment for understanding dual diagnosis if you notice that mental health symptoms and substance use challenges are linked and seem to make each other worse over time. For example, if anxiety or depression feels harder to manage when you’re using substances, or if stopping one issue causes the other to flare up, research shows that treating both at the same time leads to better outcomes than addressing just one4.
How can I help a loved one who refuses to acknowledge they need understanding dual diagnosis treatment?
Supporting a loved one who isn’t ready to acknowledge their need for understanding dual diagnosis treatment can feel incredibly tough, but you’re not alone in facing this challenge. Start by listening with empathy—judgment or pressure often makes people pull away. Instead, share your concerns using “I” statements and focus on specific changes you’ve noticed, rather than making big labels or assumptions.
What credentials should I look for in a team that specializes in understanding dual diagnosis?
When looking for a team specializing in understanding dual diagnosis, seek professionals who are trained and licensed in both mental health and substance use treatment. Ideally, your team should include a psychiatrist or psychiatric nurse practitioner, licensed therapists with experience in co-occurring disorders, and addiction counselors who work collaboratively.
Are there cultural or spiritual approaches available for understanding dual diagnosis treatment?
Yes, there are cultural and spiritual approaches available for understanding dual diagnosis treatment, and these can be an important part of your recovery journey. Many integrated programs recognize that personal beliefs, traditions, and a sense of community shape how you heal from co-occurring mental health and substance use challenges.
What is the success rate for people committed to understanding dual diagnosis recovery?
The success rate for people who commit to understanding dual diagnosis recovery is encouraging—long-term studies show that around 62% achieve remission from substance use, and nearly 58% report real satisfaction with their lives after ten years of sustained, integrated care10.
How do I transition from residential treatment to outpatient care while maintaining understanding dual diagnosis support?
Transitioning from residential treatment to outpatient care while maintaining understanding dual diagnosis support is a big step, but you don’t have to do it alone. Start by working closely with your residential care team to create a detailed aftercare plan that covers both mental health and substance use needs.
What happens if my insurance doesn’t cover integrated dual diagnosis treatment?
If your insurance doesn’t cover integrated dual diagnosis treatment, you still have options for getting support. Start by asking your provider about any appeals process—sometimes, a detailed letter from your care team explaining why integrated care is medically necessary for understanding dual diagnosis can make a difference.
Can I participate in understanding dual diagnosis treatment while keeping my job?
Yes, you can participate in understanding dual diagnosis treatment while keeping your job. Many integrated care programs offer flexible options—including intensive outpatient programs (IOPs) that provide therapy and group sessions outside of standard work hours, often in the evenings or on weekends.
How long does understanding dual diagnosis treatment typically take before I see improvement?
The timeline for seeing improvement in understanding dual diagnosis treatment can be different for everyone, but you can expect to notice some positive changes within the first few weeks—especially with integrated support that addresses both mental health and substance use at the same time.
Will my family need to be involved in my understanding dual diagnosis treatment?
Family involvement in understanding dual diagnosis treatment isn’t required, but it often helps your recovery journey feel more supported and less isolating. Many people find that when loved ones learn about co-occurring disorders and the challenges you’re facing, they become allies in your healing process.
What if I’ve tried treatment before and it didn’t work—how is understanding dual diagnosis different?
If you’ve tried treatment before and felt discouraged by the results, you’re not alone. What sets understanding dual diagnosis apart is the focus on integrated care: both conditions are addressed together, by the same team, using therapies that connect your experiences and build on your strengths.
How do I choose between partial hospitalization and intensive outpatient programs for understanding dual diagnosis?
Choosing between partial hospitalization and intensive outpatient programs for understanding dual diagnosis starts with looking at your daily needs and challenges. Partial hospitalization programs (PHPs) give you a highly structured, on-site environment—usually 20–30 hours a week—making them a good match if your symptoms feel overwhelming.
Is virtual treatment as effective as in-person care for understanding dual diagnosis?
Yes, virtual treatment can be just as effective as in-person care for understanding dual diagnosis—especially when programs are truly integrated, offer real-time support, and address both mental health and substance use together.
What role does trauma play in understanding dual diagnosis and recovery?
Trauma plays a powerful role in understanding dual diagnosis and your recovery journey. Many people experiencing both mental health and substance use challenges have a history of trauma—over 30% of adults with substance use disorders report childhood trauma, which can increase the risk for both conditions to develop together6.
Finding Hope Through Comprehensive Care
Recovery from co-occurring disorders is possible, and it begins with finding integrated treatment that addresses both conditions simultaneously. As we’ve explored throughout this article, psychiatric disorders and substance use disorders are deeply interconnected—treating one while ignoring the other leaves you vulnerable to relapse and continued suffering. Comprehensive dual diagnosis care recognizes this critical relationship and provides coordinated treatment that gives you the best chance at lasting recovery.
Effective integrated treatment combines evidence-based therapies tailored to your unique combination of mental health and substance use challenges. This might include individual counseling that addresses both conditions, group therapy with others facing similar dual diagnosis struggles, psychiatric medication management, and therapeutic approaches specifically designed for co-occurring disorders. The goal is to help you understand how your mental health and substance use influence each other while developing healthy coping strategies that support recovery from both.
What makes dual diagnosis treatment so powerful is its unified approach. Rather than shuttling between separate providers for your mental health and addiction—an approach that often leads to conflicting treatment plans and gaps in care—integrated treatment provides coordinated support under one roof. Your treatment team communicates regularly, ensuring that progress in one area reinforces gains in the other and that setbacks are addressed comprehensively.
The journey through dual diagnosis treatment is deeply personal, and there’s no one-size-fits-all solution. Quality integrated programs recognize this and create individualized care plans that address your specific combination of conditions and circumstances. From initial assessment through aftercare planning, each phase builds upon the last, creating a strong foundation for managing both your mental health and your recovery.
You don’t have to face co-occurring disorders alone. Seek out treatment providers who specialize in dual diagnosis care and understand the complex relationship between mental health and substance use. Whether you’re seeking help for yourself or a loved one, asking specifically about “dual diagnosis treatment” or “integrated care for co-occurring disorders” ensures you’ll receive the comprehensive support you need. With proper integrated treatment, both your mental health and your substance use can improve together—not just managing symptoms, but building genuine wellness and a more fulfilling future. Recovery from both conditions is within reach.
References
- Dual Diagnosis. https://medlineplus.gov/dualdiagnosis.html
- Understanding Dual Diagnosis. https://www.nami.org/Blogs/NAMI-Blog/October-2017/Understanding-Dual-Diagnosis
- Co-Occurring Disorders and Health Conditions. https://nida.nih.gov/research-topics/co-occurring-disorders-health-conditions
- Integrated vs non-integrated treatment outcomes in dual diagnosis. https://pmc.ncbi.nlm.nih/articles/PMC10157410/
- Dual Diagnosis: Double the Stigma, Double the Trouble. https://www.psychiatrictimes.com/view/dual-diagnosis-double-the-stigma-double-the-trouble
- Treatment Access Barriers and Disparities Among Individuals with Co-Occurring Disorders. https://pmc.ncbi.nlm.nih/articles/PMC4695242/
- Co-Occurring Disorders and Other Health Conditions. https://www.samhsa.gov/substance-use/treatment/co-occurring-disorders
- Working with People Who Have Co-Occurring Disorders. https://www.ncbi.nlm.nih.gov/books/NBK571013/
- Finding Help for Co-Occurring Substance Use and Mental Disorders. https://www.nimh.nih.gov/health/topics/substance-use-and-mental-health
- Ten-Year Recovery Outcomes for Clients With Co-Occurring Disorders. https://pmc.ncbi.nlm.nih/articles/PMC2632251/






