Key Takeaways for Your Decision
- Assess Your Needs: Determine if you require 24/7 supervision (residential) or if you can manage recovery while living at home (IOP).
- Verify Accreditation: Ensure your chosen program holds a current seal from The Joint Commission or CARF International.
- Prioritize Integration: Look for “Dual Diagnosis” capabilities to treat mental health and substance use simultaneously.
- Immediate Action: Call your insurance provider to verify coverage for “Intensive Outpatient” services in Montana.
Understanding What Makes an IOP Montana Program Trustworthy
Accreditation Standards That Protect You
Navigating the search for a reliable IOP Montana program can feel overwhelming, but understanding accreditation is your first line of defense. You will discover how accreditation protects you when choosing a program residents can rely on, and you will know you have learned it when you can confidently check for key certifications in any program you consider.

Imagine you are taking a road trip across Montana. You would want your car to be inspected and safe, right? That is what accreditation does for IOP Montana programs—it is a safety check for your care. Trusted organizations like The Joint Commission and CARF International review programs to make sure they meet strict standards for safety, staff training, patient rights, and effective treatment3, 4.
When an IOP Montana provider is accredited, it means experts have checked that the program follows evidence-based practices and is ready for independent audits.
Breaking Down the Basics: Look for these specific accreditations:
- The Joint Commission: Sometimes referred to as “JCAHO,” this is the gold standard in healthcare accreditation.
- CARF International: The Commission on Accreditation of Rehabilitation Facilities focuses specifically on health and human services.
An IOP Montana program with these seals has proven it offers person-centered care, protects your privacy, and keeps your health and safety first3, 4.
Practice This: Create a “Trust Checklist”
Use the following script when calling a provider:
Are you accredited by The Joint Commission or CARF?
How often is your program reviewed?
Can I see your current accreditation certificate?
Skill Checkpoint: You are ready for the next level when you can identify at least two major accrediting bodies and explain why they matter for your safety and quality of care.
Evidence-Based Therapies You Deserve
You will discover why the therapies used in an IOP Montana program matter for your recovery, and you will know you have learned it when you can name at least two evidence-based therapies and explain how they support real change.
Imagine you are building a house—you would not use random materials; you would want the strongest, most reliable ones. In the same way, a trustworthy IOP Montana program should use therapies that research shows actually work. Approaches like Cognitive Behavioral Therapy (CBT), Dialectical Behavior Therapy (DBT), and Motivational Interviewing are proven to help people reduce substance use, manage stress, and improve quality of life8.
| Therapy Type | Primary Benefit |
|---|---|
| Cognitive Behavioral Therapy (CBT) | Helps you notice and change unhelpful thoughts and actions. |
| Dialectical Behavior Therapy (DBT) | Gives you practical tools for handling tough emotions and relationships. |
| Motivational Interviewing (MI) | Encourages you to find your own internal reasons for change. |
Medication-assisted treatment (MAT) is another evidence-based option, especially for opioid use disorder. MAT has been shown to reduce overdose risk by up to 76% at three months6.
Practice This: Create a “Therapy Match List”
Write down which therapies sound right for you. Ask any IOP Montana provider which ones they offer and how they fit your needs.
Skill Checkpoint: You are ready for the next level when you can explain the difference between at least two evidence-based therapies and ask a provider about their experience using them.
Why Dual Diagnosis Integration Matters in IOP Montana
When mental health conditions and substance use disorders occur together, they create a complex web of challenges that require specialized care. Traditional treatment approaches that address only one condition often fall short because these disorders are deeply interconnected. Dual diagnosis integration matters because it recognizes this fundamental truth: you cannot effectively treat one condition while ignoring the other.
Research demonstrates that integrated dual diagnosis treatment produces significantly better outcomes than treating each condition separately. Studies show that integrated treatment approaches reduce relapse rates by 30-50% compared to sequential or parallel treatment models.
When mental health symptoms go unaddressed during substance use treatment, they often trigger relapse. Similarly, continuing substance use undermines mental health treatment progress. Consider how this plays out in real life: when anxiety triggers substance use as a coping mechanism, which then disrupts sleep and worsens depression, which increases anxiety—creating a downward spiral that single-focus treatment cannot effectively interrupt. An integrated approach breaks this cycle by addressing both conditions simultaneously through coordinated care.
The integration of dual diagnosis treatment creates a more complete understanding of your unique situation. Mental health professionals and addiction specialists work together, sharing insights and developing treatment strategies that account for how your conditions interact. This collaborative approach means you receive consistent messages and interventions that support your overall recovery, rather than conflicting advice from separate providers.
Dual diagnosis integration also improves treatment efficiency and reduces the burden on you as someone seeking help. Instead of navigating multiple treatment systems, attending separate appointments, and trying to coordinate your own care, integrated programs streamline the process. You work with a unified treatment team that communicates regularly and adjusts your care plan based on your progress across all areas of recovery.
This comprehensive approach also enables you to develop coping strategies that address both mental health symptoms and substance use triggers simultaneously. You learn holistic skills that prepare you for real-world situations where both challenges may arise together, giving you practical tools for managing co-occurring conditions in daily life.
The importance of dual diagnosis integration extends beyond immediate treatment outcomes. Integrated care reduces the likelihood of future hospitalizations, emergency room visits, and treatment readmissions. By addressing the root causes of both conditions and their interconnections, you build a stronger foundation for long-term recovery and improved quality of life.
Perhaps most importantly, dual diagnosis integration validates your complete experience. Rather than feeling fragmented between different treatment systems or having parts of your struggle dismissed, integrated care acknowledges the full complexity of co-occurring disorders. This comprehensive recognition creates a treatment environment where you feel understood, supported, and empowered to work toward lasting recovery from both conditions.
Evaluating Provider Qualifications in Montana
Staff Credentials and Training to Verify
You will understand which staff credentials and training signal a quality IOP Montana program, and you will know you have learned it when you can ask about licensure, clinical experience, and continuing education with confidence.
Think of your care team as the guide and safety crew for a mountain hike—having the right training and certifications makes your journey safer and more effective. In a trustworthy IOP Montana program, you deserve to see the following professionals:
- LACs: Licensed Addiction Counselors
- LCSWs: Licensed Clinical Social Workers
- LPCs: Licensed Professional Counselors
- Medical Staff: Board-certified physicians or nurse practitioners
These credentials show that staff have met rigorous state or national standards for education, ethics, and supervised experience. But credentials alone are not enough. Ongoing training in evidence-based therapies, crisis management, and dual diagnosis care is key. Programs that invest in regular staff training can nearly quadruple their ability to treat both substance use and mental health together—from just 11% to 48% dual diagnosis capability in 18 months9.
Practice This: Create a “Staff Qualifications Checklist”
Write down questions to ask any IOP Montana provider:
What licenses and certifications do your clinicians hold?
How often do they complete continuing education?
Are staff specifically trained in dual diagnosis or trauma-informed care?
Skill Checkpoint: You are ready to move forward when you can verify at least two staff credentials and ask how ongoing training is prioritized.
Cultural Competency and Specialized Care
You will see why cultural competency and specialized care are vital in choosing an IOP Montana program you can trust. You will know you have learned it when you can spot the ways a provider respects your background and offers care for your specific needs.
Imagine walking into a room where people value your story, traditions, and beliefs. That is the difference cultural competency makes—it means staff understand and honor your unique identity, whether it is shaped by race, faith, rural living, or tribal heritage. When an IOP Montana program is culturally competent, clients are more likely to feel understood, stay engaged, and reach their goals5.
Specialized care also matters because every person’s path to recovery is different. For example, you might need trauma-informed therapy, support for LGBTQ+ identities, or help with chronic pain. The best IOP Montana programs offer individualized services, not just a “one-size-fits-all” approach. The latest guidelines stress the importance of person-centered care—matching treatment to your social, cultural, and medical needs5.
Practice This: Create a “Personal Fit List”
Write down anything about your background or challenges that is important to your healing. Ask the IOP Montana provider how their team is trained in cultural competency and if they have experience helping people with your specific needs.
Skill Checkpoint: You are ready to move ahead when you can describe what cultural competency means and ask a provider how they will honor your unique story.
Flexible IOP Montana Treatment Options for Your Lifestyle
In-Person vs Virtual IOP Montana Programs
You will understand the key differences between in-person and virtual IOP Montana programs, and you will know you have learned it when you can decide which option is a better fit for your lifestyle and recovery needs.
Choosing between in-person and virtual IOP Montana programs is a bit like deciding whether to hike a local trail or join a guided online fitness class—both can get you moving forward, but the experience and support style feel different.
| Feature | In-Person IOP | Virtual IOP |
|---|---|---|
| Interaction | Face-to-face support and real-time group connections. | Digital connection via secure video platforms. |
| Structure | Provides a physical routine that can be grounding. | Offers flexibility for those with tight schedules. |
| Best For | Those who thrive on structure or live nearby. | Rural residents or those with transport/childcare issues. |
Montana’s vast geography means virtual care can bridge big gaps—hundreds of new telehealth IOPs launched recently to meet this need1.
Practice This: Create a “Fit Finder List”
Write down your biggest daily obstacles—like long commutes, weather, work, or family duties. Ask each IOP Montana provider if they offer both in-person and virtual options, and how they help you stay connected in either format.
Skill Checkpoint: You are ready to move on when you can list two benefits and one challenge of each IOP Montana program style, and choose the one that fits your life best.
Scheduling That Fits Your Responsibilities
You will discover how IOP Montana programs can offer flexible scheduling to match your work, family, or school commitments. You will know you have learned it when you can identify what kind of session times work best for you and confidently ask a provider about their options.
Picture your week as a puzzle—every piece, like your job shifts, family meals, or classes, needs to fit together. Finding an IOP Montana program with options for morning, afternoon, evening, or weekend sessions can make it possible to keep your commitments while building a healthier future. Programs guided by the latest ASAM Criteria now prioritize person-centered scheduling, meaning you are not expected to put your life on pause just to get help5.
Getting the Right Fit: Some IOP Montana providers offer tracks for students, parents, or working adults, and many allow you to adjust your schedule if life changes. This kind of flexibility helps people stay in treatment longer and get better results7.
Practice This: Build a “Schedule Wish List”
Write down your busiest times and most important responsibilities. When you talk to an IOP Montana provider, ask how they will help you fit sessions into your real life.
Skill Checkpoint: You are ready for the next step when you can name your top three scheduling needs and ask about customized session options.
Frequently Asked Questions
How long should I expect to participate in an IOP Montana program?
Most people participate in an IOP Montana program for about 8 to 12 weeks, but your exact length can vary. You’ll typically attend sessions multiple times per week, with the schedule adjusted to your needs and progress. This flexible approach means some people may finish a little sooner, while others benefit from a longer stay for extra support. The latest ASAM Criteria recommend that treatment plans be tailored to your unique situation—there’s no single timeline that fits everyone 5. You’ll know you’re ready to “step down” when you’ve built strong coping skills and feel confident managing challenges outside the program.
Will my insurance cover an IOP Montana residents can access?
Many insurance plans do cover IOP Montana services, especially when the program is accredited and follows evidence-based care. Medicaid, Medicare, and most private insurance policies recognize IOP Montana as a covered level of care when medically necessary 5. To be sure, call your insurance provider and ask about your behavioral health benefits for IOP Montana programs—be ready to share the program’s accreditation and any referral or assessment paperwork. If you have Medicaid, expanded coverage in Montana now includes more outpatient options than before 3. Your IOP Montana provider can often help you verify coverage and answer questions about the process.
What happens if I need medication-assisted treatment during my IOP?
If you need medication-assisted treatment (MAT) during your IOP Montana program, your care team will work with you to include safe, effective medications—like buprenorphine or methadone—alongside counseling and group support. MAT is proven to lower overdose risk by up to 76% at three months for people with opioid use disorder 6. Your IOP Montana provider will likely coordinate with a medical professional who can prescribe and monitor your medication, ensuring you get both the medical and emotional support you deserve. Open communication about your needs helps your team adjust your plan and keep your recovery on track.
Can I switch between in-person and virtual IOP Montana sessions?
Yes, many IOP Montana programs now let you switch between in-person and virtual sessions. This flexibility helps you keep up with your recovery even when life changes—like a new job, family needs, or weather challenges. Montana’s wide-open spaces mean that virtual IOP Montana options are especially valuable, and many providers offer both formats to fit your lifestyle 1. Always ask your IOP Montana provider about their policies for switching formats and how they’ll support you in staying connected with your care team. Open communication makes it easier to find the right mix for your needs.
How do I know if I need an IOP Montana program or a higher level of care?
Deciding between an IOP Montana program and a higher level of care comes down to your current symptoms, safety, and daily functioning. If you’re managing responsibilities at home or work and don’t need 24-hour supervision, IOP Montana could be a good fit. However, you may need inpatient or residential care if you have severe withdrawal symptoms, safety concerns, or trouble coping without constant support. The ASAM Criteria recommend a thorough, person-centered assessment to match you with the right level of care—so always ask your provider how they determine placement for your needs 5.
What should I do if my previous treatment didn’t address both my mental health and substance use?
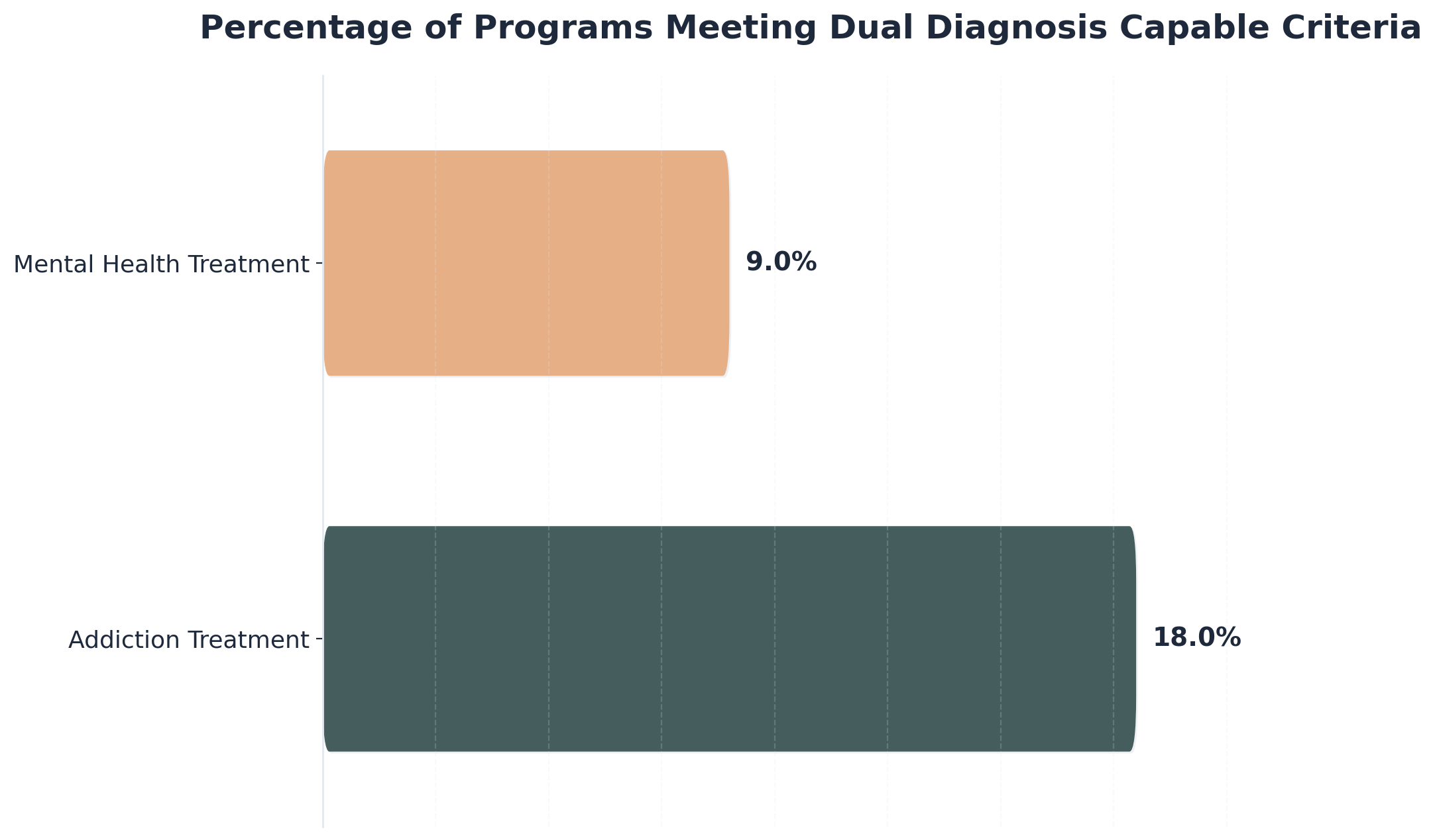
If your previous treatment didn’t address both your mental health and substance use, you’re not alone—and there is a way forward. Only about 18% of addiction treatment programs and 9% of mental health programs are truly equipped to treat both conditions at the same time, which means many people have had similar experiences 9. The best next step is to seek out an IOP Montana program that offers integrated dual diagnosis care, where both your mental health and substance use needs are treated together. Ask any IOP Montana provider about their approach to dual diagnosis, staff training, and how they’ll support your whole recovery journey.
Your Path to Recovery Starts Here
Now that you understand why integrated treatment matters, let’s talk about how you can actually begin this journey. Taking the first step toward healing from co-occurring mental health and substance use disorders requires courage, but you do not have to face this journey alone—and knowing where to start makes all the difference.

Here are the concrete steps to launch your recovery with dual diagnosis integration:
- Start by seeking a comprehensive assessment. Look for providers who evaluate both your mental health and substance use patterns together, not separately. This initial evaluation creates the foundation for everything that follows.
- Research programs with integrated treatment teams. The most effective programs have psychiatrists, therapists, and addiction specialists who work together in the same setting, communicating regularly about your progress.
- Ask potential providers specific questions about their dual diagnosis experience. How long have they been treating co-occurring disorders? What does their coordination process look like? Can they share success stories similar to your situation?
In your first weeks of integrated treatment, expect to meet with multiple specialists who will collaborate on your personalized plan. You will likely attend individual therapy, group sessions, and medication management appointments—all designed to work together seamlessly. Your treatment team will help you understand the connections between your conditions and develop coping strategies that address both simultaneously. This coordinated approach means fewer gaps in care and more consistent support as you work toward wellness.
You deserve treatment that sees the complete picture of your health. Take the next step today: reach out to a dual diagnosis program, schedule that comprehensive assessment, and begin building the integrated support system that will carry you toward lasting recovery. Your path to wellness starts with this single, courageous decision.
References
- The Effectiveness of Medication-Based Treatment for Opioid Use Disorder. https://www.ncbi.nlm.nih.gov/books/NBK541393/
- Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition Text Revision (DSM-5-TR). https://www.americanpsychiatry.org/psychiatrists/practice/dsm
- The Joint Commission – Accreditation Standards for Healthcare. https://www.jointcommission.org/en/
- CARF International – Accreditation for Health and Human Services. https://www.carf.org/
- ASAM Criteria, Fourth Edition – Patient Placement and Level of Care Standards. https://www.asam.org/asam-criteria
- Comparative Effectiveness of Different Treatment Pathways for Opioid Use Disorder. https://jamanetwork.com/journals/jamanetworkopen/fullarticle/2760032
- National Institute on Drug Abuse – Treatment and Recovery Resources. https://nida.nih.gov/research-topics/treatment-recovery
- SAMHSA Evidence-Based Practices Resource Center. https://www.samhsa.gov/libraries/evidence-based-practices-resource-center
- Dual Diagnosis Capability in Addiction Treatment and Mental Health Programs. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3594447/
- Settings, Levels of Care, and Patient Placement in Addiction Treatment. https://www.ncbi.nlm.nih.gov/books/NBK64109/






