Key Takeaways
- Definition: Experiential therapy is a therapeutic approach that uses expressive tools and activities to help patients process emotions through action rather than just words.
- Core Benefits:
- Bypasses verbal defense mechanisms to access deep-seated trauma.
- Utilizes the “felt sense” to connect physical sensations with emotional states.
- Creates new neural pathways through active engagement and role-play.
- Target Audience: This modality is particularly effective for individuals with co-occurring disorders who find traditional talk therapy limited or difficult to access emotionally.
What Experiential Therapy Means Today
Beyond Traditional Talk-Based Methods
You are likely familiar with the standard clinical setting: two people sitting in a room, discussing memories, analyzing thoughts, and building insight through conversation. While valuable, this format has limitations, particularly when trauma or deep-seated addiction patterns are involved. Experiential therapy diverges from this path by prioritizing action over analysis. Instead of solely discussing your history, you actively engage in experiences—creating art, role-playing scenarios, or interacting with the environment.
Consider the difference between reading a manual on aerodynamics and actually piloting a plane. You can understand the theory of flight perfectly, but the physical reality of flying requires a different set of skills. Similarly, experiential therapy allows you to “do” recovery rather than just “discuss” it. This is crucial because trauma often resides in parts of the brain that language cannot easily reach.
“Research shows that for many, especially those recovering from substance use or trauma, emotions and memories can be hard to put into words. During intense moments, the parts of the brain that handle speech can actually slow down, making verbal sharing difficult.”8
By engaging in experiential therapy, you bypass the verbal blockages. You express feelings and process pain through movement and creation, often achieving breakthroughs that talk therapy might take years to uncover. Evidence suggests that these dynamic therapies show strong, lasting effects for trauma and addiction, often outpacing standard methods in long-term efficacy7.
The Felt Sense and Body-Based Healing
Healing is not just a cognitive process; it is a physiological one. You may have experienced the “felt sense”—those subtle, somatic signals that precede conscious thought. This might manifest as:
- A tightening in the chest when discussing family dynamics.
- A heaviness in the stomach associated with grief.
- A restless energy in the limbs when recalling a craving.
Experiential therapy excels at tuning into these signals. Rather than ignoring the body to focus on the mind, this approach guides you to notice how your body reacts during hands-on activities. By paying attention to these physical cues during art-making or movement, you access emotions buried beneath the surface of your conscious narrative.
It can be uncomfortable to sit with these sensations, but this awareness is where true progress begins. Research highlights that profound change often starts with this bodily awareness—meaning starts in the viscera and only later becomes something you can articulate10. Through experiential therapy, you build trust in your own physical experience, creating a safer internal environment for recovery.
How Experiential Therapy Works
Accessing Trauma Through Non-Verbal Pathways
When trauma occurs, the brain’s Broca’s area—responsible for speech—often shuts down, while the amygdala—the alarm center—flares up. This is why you might struggle to describe a traumatic event even if you want to heal. Experiential therapy offers a workaround. It utilizes non-verbal pathways to process pain, effectively turning up the volume on your internal experience without requiring you to find the perfect words immediately.
Unlike traditional therapy which moves from Cognition to Emotion, experiential methods start with Action to unlock the rest.
Think of this as trying to describe a complex symphony using only mathematical equations; you miss the emotional resonance. Experiential therapy allows you to “play the music” of your experience through psychodrama or art. These activities bypass verbal defenses, allowing you to express the unspeakable. Research indicates that action-based approaches allow survivors to process experiences when talking alone is insufficient, giving a voice to pain that has been locked away8.
Clinical Note: Managing Intensity
Because these pathways are direct, the emotional release can be intense. It is normal to feel vulnerable. However, every creative step or movement is a meaningful release of stored pressure, facilitating deep healing.
Creating New Neural Patterns Through Action
Lasting recovery requires neuroplasticity—the brain’s ability to reorganize itself by forming new neural connections. Experiential therapy leverages this by moving beyond theory into practice. Instead of discussing how you should react to stress, you practice new reactions in a safe, controlled environment. Each time you engage in a therapeutic action, you are physically wiring your brain for a new response.
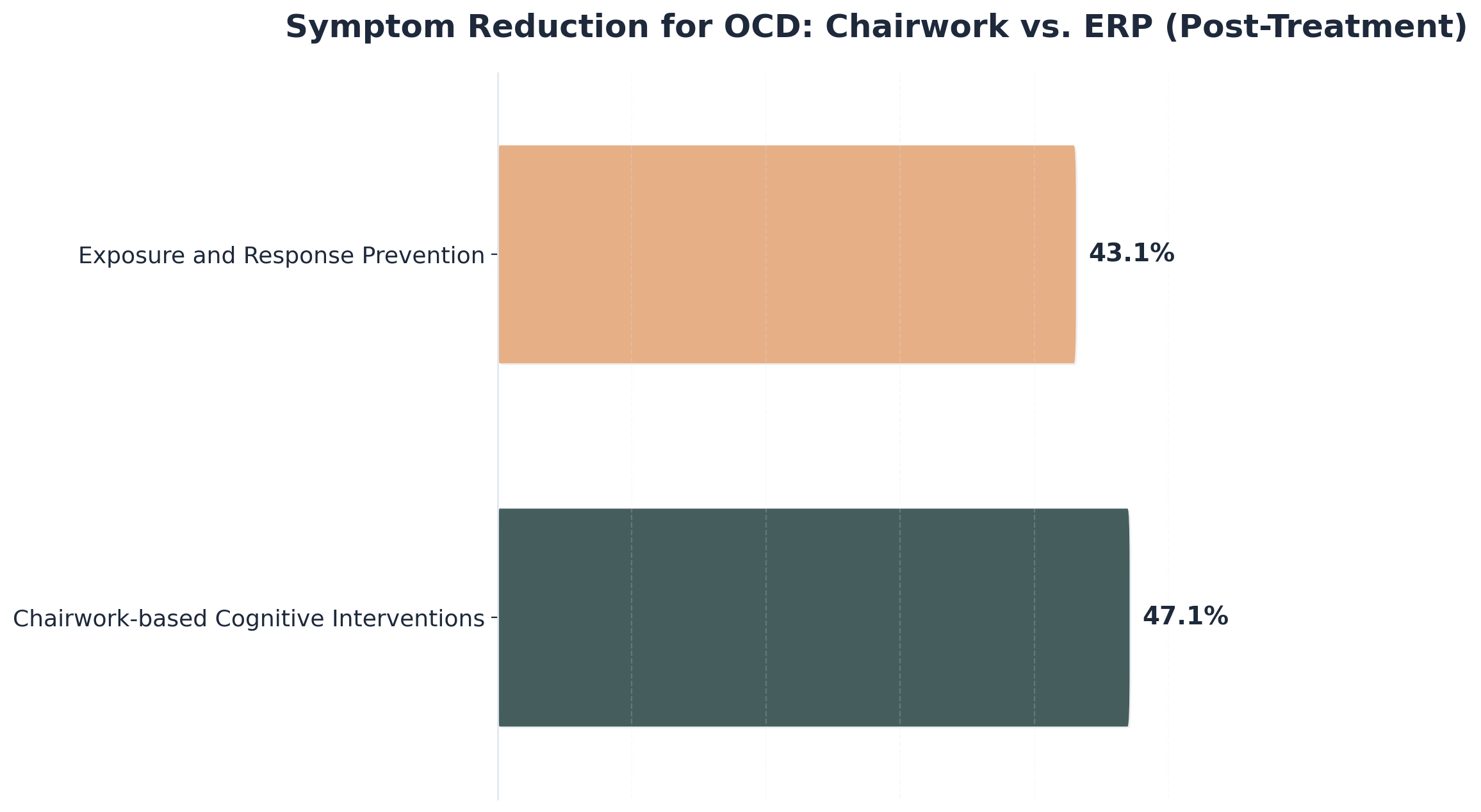
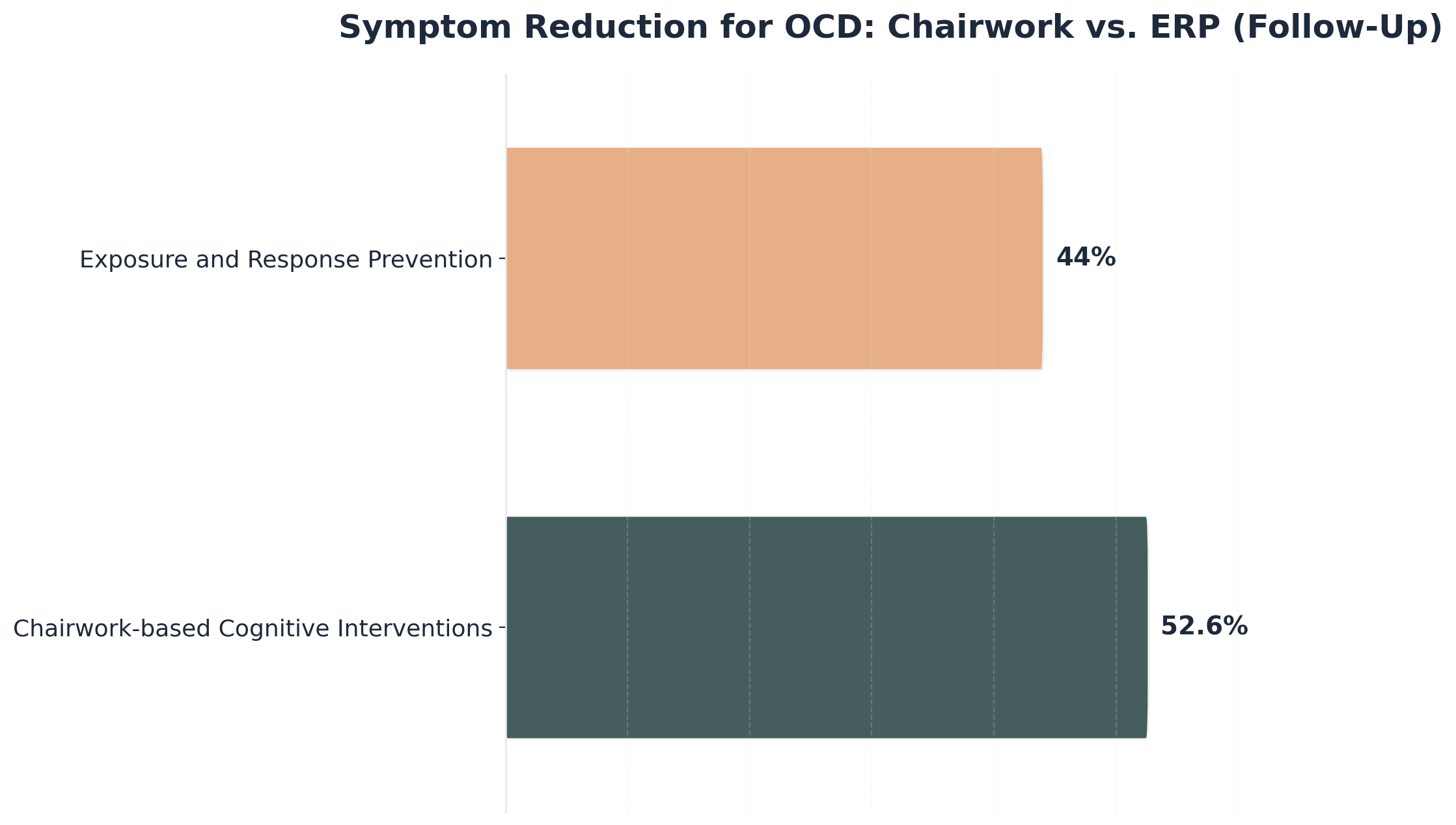
Imagine walking through a dense forest. The first time you carve a path, it is difficult. But the more you walk it, the clearer and easier it becomes. Old patterns—like isolation or substance use—are replaced by healthier responses as you rehearse them during experiential therapy. Research supports this, showing that action-based interventions like chairwork can lead to greater symptom reduction than some traditional methods over time1.
Building these new patterns takes courage. It may feel slow, but every action is a signal to your brain that change is possible. As you continue with experiential therapy, these new neural pathways strengthen, making recovery behaviors feel more natural and automatic.
Core Modalities in Experiential Therapy
Creative Arts and Expression-Based Approaches
Creative arts are perhaps the most visible forms of experiential therapy. These modalities provide a canvas or a stage where you can externalize internal conflicts. Whether it is drumming to release anger or painting a representation of your grief, these activities provide a container for feelings that are too complex for conversation.
| Modality | Primary Mechanism | Key Benefit |
|---|---|---|
| Music Therapy | Rhythm and lyric analysis | Lowers anxiety, regulates heart rate, aids emotional release3. |
| Art Therapy | Visual creation (painting, sculpture) | Processes trauma non-verbally, visualizes hope and recovery. |
| Psychodrama | Role-playing and enactment | Improves communication skills, allows “re-do” of past conflicts6. |
Research confirms that music therapy can significantly lower anxiety and depression while boosting positive emotions. Similarly, drama-based methods allow you to role-play parts of your life, giving voice to experiences that have been silenced. Experiential therapy using these arts makes the healing process adaptable and engaging, regardless of your artistic ability.
Nature-Based and Animal-Assisted Methods
Stepping out of the clinical office and into nature brings a refreshing dimension to experiential therapy. Nature-based therapy uses the environment as a co-therapist. Activities like gardening, wilderness walks, or adventure therapy help you reconnect with your senses and reduce cortisol levels. Research finds that spending time in nature during therapy improves motivation and decreases depression, creating a sense of safety that facilitates openness9.
Animal-assisted therapy, particularly equine therapy, adds a relational layer to experiential therapy. Horses are highly sensitive to non-verbal cues and emotional states. Working with them requires you to be grounded, authentic, and calm.
For example, if you approach a horse with high anxiety or aggression, the animal will react instantly, providing immediate, non-judgmental feedback. This interaction helps you practice emotional regulation and boundary setting in real-time. Studies show that equine-assisted therapy is particularly effective for improving self-esteem and emotion regulation in those with substance use disorders5.
Evidence and Outcomes for Dual Diagnosis
When addressing co-occurring disorders—where substance use and mental health challenges exist simultaneously—experiential therapy serves as a critical bridge. Clinical research consistently demonstrates that integrated treatment approaches produce significantly better outcomes than treating conditions separately. Experiential therapy is vital here because it addresses the underlying emotional dysregulation that fuels both addiction and mental health symptoms.
Patients engaged in experiential therapy within a dual diagnosis framework often demonstrate higher rates of sustained sobriety and improved functioning. By addressing the “whole person” through action-based methods, you are not just managing symptoms but resolving the root causes. One landmark study found that integrated treatment reduced substance use by 40% and psychiatric symptoms by 35% compared to sequential approaches.
“Research shows retention rates improve by 25-30% when mental health and addiction are treated concurrently. This improvement likely reflects the stabilizing effect of addressing co-occurring symptoms.”
Furthermore, experiential therapy enhances the efficacy of other evidence-based modalities like CBT and DBT. While CBT helps identify cognitive distortions, experiential methods provide the “lab” to test new behaviors. This combination reduces relapse rates significantly. Long-term data suggests that individuals who engage in experiential therapy maintain improvements in quality of life and interpersonal functioning years after treatment concludes.
Trauma-informed experiential therapy is particularly promising for dual diagnosis. By processing trauma without re-traumatizing the client through forced verbalization, these methods help build the resilience necessary for long-term recovery. When you address the etiological factors contributing to co-occurring disorders through experience, you achieve more sustainable outcomes.
Frequently Asked Questions
Is experiential therapy right for everyone seeking substance use treatment?
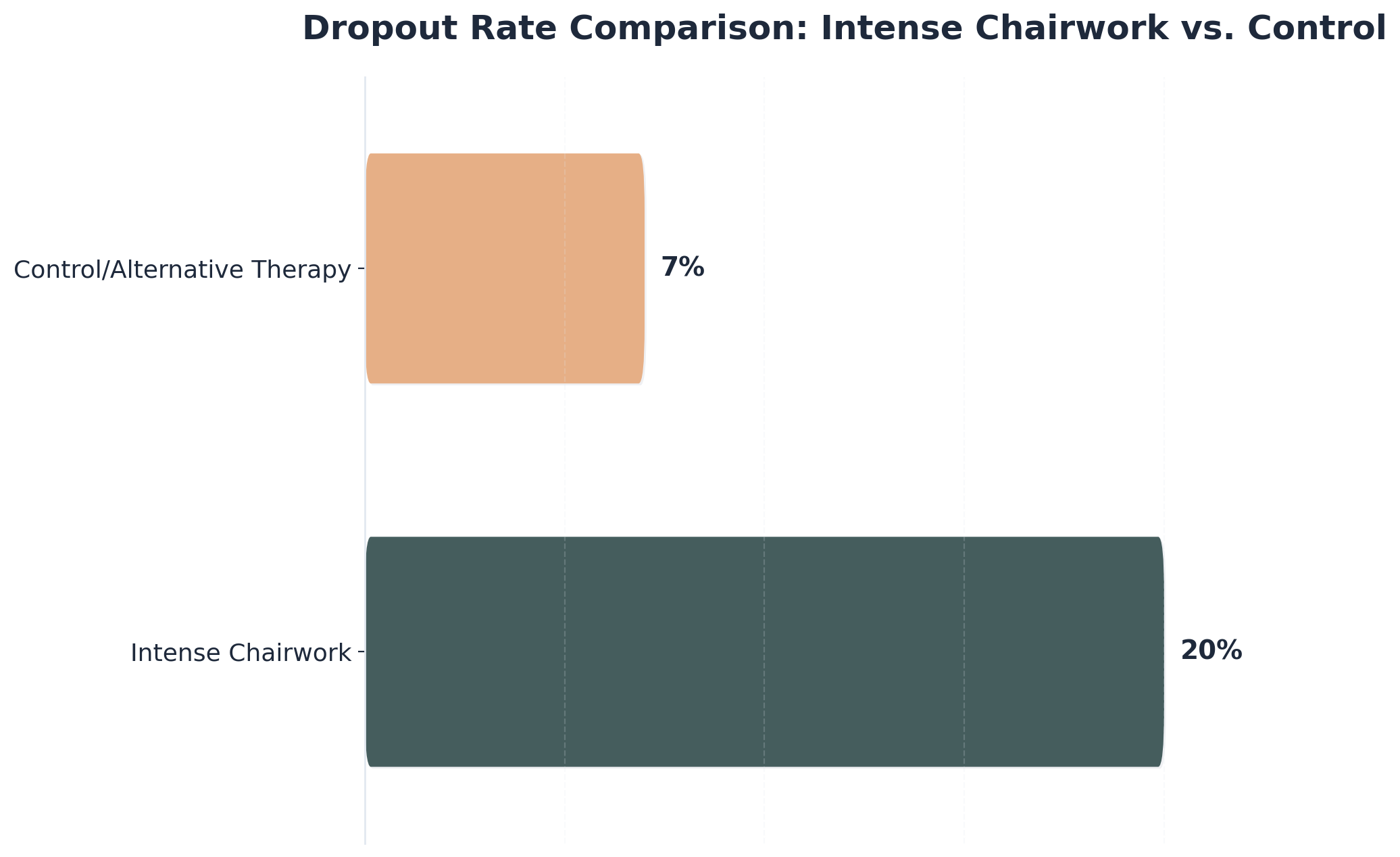
Experiential therapy can be a powerful tool for many people seeking substance use treatment, but it isn’t always the right fit for everyone. Some individuals, such as those experiencing active psychosis or with certain physical limitations, may not benefit or could even feel overwhelmed by the intensity of some experiential methods 1. Research also shows that emotionally intense techniques can lead to higher dropout rates—about 20% for some approaches compared to 7% for standard therapies—so careful assessment is important 1. Yes, these challenges are real, but with proper support, most people tolerate experiential therapy well. Every person’s journey is unique, and matching the approach to the individual’s readiness and needs is key to making progress.
Can experiential therapy be delivered virtually or does it require in-person participation?
Experiential therapy can be delivered both in-person and virtually, depending on the approach and the needs of each participant. Some methods—like art, music, drama, and certain mindfulness activities—work well through video sessions or digital platforms. Virtual experiential therapy has grown rapidly, making these services more accessible for people who can’t attend in person due to distance, mobility, or other barriers 7. However, activities that involve physical space, nature, or animal-assisted methods are best suited for in-person settings. Each mode offers its own strengths: virtual sessions provide flexibility and reach, while in-person experiences can deepen connection and engagement.
How long do the benefits of experiential therapy last after treatment ends?
The benefits of experiential therapy can last well beyond the end of treatment, especially for those dealing with substance use and mental health challenges. Research shows that positive changes—like improved emotion regulation and reduced cravings—often remain strong over the long term, with some effects even growing after therapy ends 7. For example, meta-analyses found that people who completed experiential dynamic therapies continued to see significant progress at follow-up, compared to those who only received inactive or standard treatments. Of course, ongoing support or participation in aftercare can help maintain these gains, as some experiential methods may need reinforcement to keep benefits going 4.
What happens if someone finds experiential therapy too emotionally intense?
If someone finds experiential therapy too emotionally intense, it’s important to pause and honor those feelings. Some activities, like chairwork or deep role-play, can stir up strong emotions and even lead to overwhelm for about 20% of participants—much higher than standard therapy approaches 1. When this happens, slowing down or switching to less intense methods can help. Checking in regularly, creating breaks, or offering extra support can make sessions feel safer. Remember, feeling overwhelmed is not a failure; it often signals real progress. Every time someone voices their discomfort and takes a break, that’s a step forward in their healing.
How does experiential therapy differ from traditional cognitive behavioral therapy?
Experiential therapy stands apart from traditional cognitive behavioral therapy (CBT) by making hands-on experiences the center of the healing process. While CBT focuses on identifying and changing unhelpful thoughts through structured talk and mental exercises, experiential therapy gets people actively involved in activities like art, role-play, or movement. Imagine the difference between reading about swimming and actually jumping in the pool—experiential therapy is about “doing” instead of just talking. Research shows that these action-based approaches can reach emotions and memories that may stay out of reach with words alone, especially for trauma and substance use 8.
Can experiential therapy be combined with medication-assisted treatment?
Yes, experiential therapy can be combined with medication-assisted treatment (MAT) for individuals working through substance use and mental health challenges. This blended approach lets you address both the biological and emotional sides of recovery. While MAT helps manage cravings and physical symptoms, experiential therapy provides hands-on ways to process emotions, practice new coping skills, and rebuild confidence. Research supports using experiential therapy alongside other evidence-based treatments to achieve better overall outcomes for clients with complex needs 7. Combining these methods gives people a fuller toolkit for healing—one that honors both their body and their lived experience.
Conclusion
The integration of experiential therapy into dual diagnosis treatment represents a significant advancement in how we approach recovery. By addressing mental health and substance use disorders simultaneously through coordinated, action-oriented care, you are positioned for better outcomes—including higher retention rates and reduced relapse incidents.
For you as a professional or a peer in this journey, understanding the value of experiential therapy is more than academic—it is practical. The research consistently shows that integrated models utilizing these dynamic methods outperform sequential treatment structures. Programs that adopt comprehensive experiential therapy protocols report improved engagement and better long-term success.
The clinical implications are clear: co-occurring disorders require simultaneous intervention because the conditions are neurologically interconnected. Addressing substance use without treating the underlying trauma via experiential therapy leaves you vulnerable. Integrated treatment provides the comprehensive framework necessary for sustainable recovery.
As the field evolves, experiential therapy continues to prove its worth, offering a robust path for those with complex needs. It is an invitation to move beyond just talking about healing and to start living it, ensuring that your recovery is as deep and resilient as you are.
References
- Experiential therapies including Chairwork: a systematic review. https://pmc.ncbi.nlm.nih.gov/articles/PMC12876151/
- Written Exposure Therapy for PTSD. https://www.ptsd.va.gov/professional/treat/txessentials/written_exposure_therapy.asp
- The Use of Art and Music Therapy in Substance Abuse Treatment. https://pmc.ncbi.nlm.nih.gov/articles/PMC4268880/
- The effectiveness of wilderness and adventure therapy programmes. https://youthendowmentfund.org.uk/wp-content/uploads/2025/09/Wilderness-therapy-effects-on-ASB-and-offending_A-systematic-review.pdf
- Equine-assisted therapy effectiveness in improving emotion regulation in substance use disorder patients. https://pmc.ncbi.nlm.nih.gov/articles/PMC10576391/
- Effectiveness of Drama-Based Intervention in Improving Mental Health. https://pmc.ncbi.nlm.nih.gov/articles/PMC10048456/
- The Efficacy of Experiential Dynamic Therapies: A 10‐Year Systematic Review and Meta‐Analysis Update. https://pmc.ncbi.nlm.nih.gov/articles/PMC12102587/
- Psychodrama as an effective treatment for trauma and PTSD. https://www.apadivisions.org/division-49/news-events/psychodrama-trauma-treatment
- Nature-Based Therapy in Individuals with Mental Health Disorders. https://pmc.ncbi.nlm.nih.gov/articles/PMC9914984/
- Experiential Therapy. https://neupsykey.com/experiential-therapy/






