Key Takeaways
- Decision Flowchart: Assess symptom overlap → Consult a multidisciplinary team → Select integrated dual diagnosis services.
- Top 3 Success Factors: Consistent attendance (aim for 90%+ engagement), active participation in evidence-based therapies (like CBT or DBT), and building a robust support network.
- Immediate Next Action: Schedule a comprehensive clinical assessment to map out your personalized treatment timeline and resource requirements.
Why Integrated Care in Dual Diagnosis Services Changes Everything
How Co-Occurring Conditions Interact
As a professional, you understand that operational efficiency requires addressing root causes. When substance use and mental health challenges appear together, they don’t just overlap—they compound one another, impacting both personal well-being and professional performance. Seeking specialized dual diagnosis services is the most effective strategy to break this cycle.
Checklist: Recognizing Interaction Between Substance Use and Mental Health Conditions
- Does substance use change the intensity or frequency of mental health symptoms?
- Are mood swings, anxiety, or paranoia tied to periods of use or withdrawal?
- Have mental health symptoms led to increased substance use as a coping strategy?
- Do both issues seem to worsen when addressed separately?
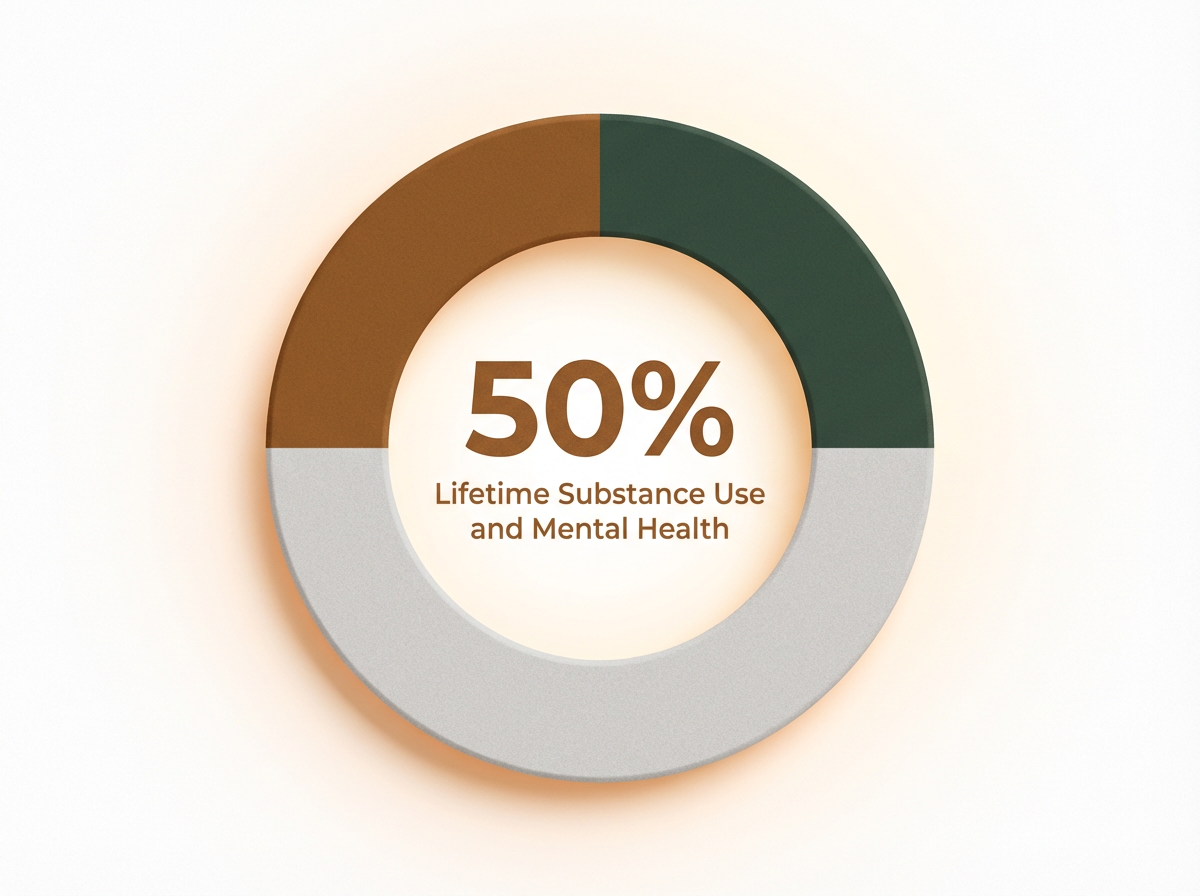
Roughly half of all people with a substance use disorder will also experience a mental health disorder at some point in their lives, highlighting how common and intertwined these conditions are1. Treating only one side often leads to setbacks, since the untreated condition can trigger relapse or worsening symptoms.
“Dual diagnosis services give you a plan to untangle these patterns, making it possible to move forward, even when progress feels slow.”
Every small victory matters, and understanding how these conditions interact is the first step toward lasting change. Next, you’ll see why treating both conditions together offers real advantages over single-focus care.
The Integrated Treatment Advantage
Decision Tool: When Does Integrated Treatment Make Sense?
- Are both mental health and substance use symptoms present and persistent?
- Have single-focus treatments failed to produce lasting change?
- Do you notice setbacks when only one condition is addressed?
- Is there a need for coordinated medication and therapy support?
You know firsthand that traditional, one-sided approaches often miss the mark when it comes to co-occurring conditions. Integrated care means treating both mental health and substance use disorders at the same time, using a team-based model. Consider this method if you are seeing patterns that overlap or worsen one another, making single-focus care ineffective or even risky.
Integrated teams can include therapists, prescribers, and peer support—everyone working together to keep your plan consistent and supportive. Research consistently shows that dual diagnosis services deliver stronger results than separate treatments. People in integrated programs have higher treatment retention and better long-term outcomes, especially when both medication and behavioral therapies are coordinated in real time3.
Yes, it takes extra coordination, and there’s no quick fix. But every bit of progress is a win, and integrated care is designed to help you build on those wins, even when things feel tough. Next, you’ll get a closer look at how these programs are structured for success.
Core Components of Effective Dual Diagnosis Services
Comprehensive Assessment and Planning
Assessment Blueprint: What Does a Dual Diagnosis Evaluation Cover?
| Assessment Area | Clinical Focus |
|---|---|
| Substance Use & Mental Health | History, current patterns, symptoms, diagnoses, and past treatments. |
| Physical Health | Physical health check (including labs, if needed). |
| Background & Risk Factors | Family, social, cultural background, suicidality, trauma, and housing instability. |
| Strengths & Support | Coping skills, resilience factors, and existing support networks. |
Comprehensive assessment is the first step in any effective dual diagnosis services plan. You know how quickly symptoms can blur together—so a thorough evaluation doesn’t just tick boxes, it creates a strategic map for treatment. This process looks at substance use and mental health in detail, making sure nothing is overlooked.
It’s normal for this to take a few hours and involve several team members. For example, you might meet with a therapist, a medical provider, and sometimes a peer specialist to get a full picture of needs and strengths. This approach works best when you’re facing overlapping symptoms, uncertain diagnoses, or previous treatment failures.
A detailed plan emerges from these findings, outlining therapy types, medication strategies, and support resources tailored for you. Resource needs include a multidisciplinary team and access to medical, psychological, and social supports—often requiring 3–5 hours of staff time up front to get it right. Thorough assessment and planning set the stage for better retention and outcomes3. Every bit of clarity you gain here becomes a tool for the journey ahead.
Evidence-Based Therapeutic Approaches
Therapy Selector: Matching Interventions to Needs
- Cognitive Behavioral Therapy (CBT): Effective for both substance use and a range of mental health symptoms, helping you challenge negative thinking and build practical coping skills.
- Dialectical Behavioral Therapy (DBT): Especially helpful for emotional regulation and reducing self-harm or impulsive behaviors.
- Motivational Interviewing (MI): Supports readiness for change and boosts your confidence to take the next step.
- Trauma-Informed Approaches: Prioritize safety, trust, and empowerment if past trauma shapes current struggles.
- Peer Support and Psychoeducation: Offer connection, shared experience, and practical knowledge for daily challenges.
Evidence-based therapies anchor dual diagnosis services, providing stability when things feel unpredictable. These approaches are backed by research showing improved retention, reduced relapse, and stronger quality of life when applied together3, 4. CBT and DBT often require a time investment of 12–24 sessions to see measurable gains.
MI may involve a few focused meetings, while trauma-focused care and peer support vary by individual needs and recovery speed. This strategy suits professionals who present with complex symptoms, or when prior attempts at single-focus therapy haven’t stuck. You might need a multidisciplinary team trained in multiple evidence-based models, along with regular supervision and ongoing staff training.
Time and effort will add up, but every breakthrough—no matter how small—moves you closer to whole-person healing. Next, you’ll explore how different program formats and flexible options can support your progress.
Treatment Formats and Flexibility Options
Structured In-Person Programs
Program Checklist: What to Expect in Structured In-Person Dual Diagnosis Services
- Daily or multi-day attendance at a treatment center
- Scheduled individual and group therapy sessions
- On-site access to medical and psychiatric care
- Medication management and monitoring
- Skills-building activities, wellness groups, and peer support
- Regular progress reviews with your treatment team
Structured in-person programs give you a predictable routine and a supportive environment where healing feels possible, even on tough days. These settings typically include Partial Hospitalization Programs (PHP) or Intensive Outpatient Programs (IOP), each with clear expectations for participation and safety. You’ll find a mix of evidence-based therapies, from Cognitive Behavioral Therapy (CBT) to trauma-informed groups, in addition to opportunities for creative expression and physical wellness.
Opt for this framework when you need consistent, face-to-face support—especially if home isn’t a stable or substance-free space. The daily structure helps you practice new habits while surrounded by professionals who understand the ups and downs of co-occurring recovery.
Most structured in-person dual diagnosis services require a commitment of 15–30 hours per week for several weeks or months, with a multidisciplinary team guiding your progress3. Yes, it’s a big investment of time and energy, but every day you show up is a step forward. Next, you’ll see how virtual care can extend support beyond the walls of a treatment center.
Virtual Care and Accessibility
Accessibility Assessment: Is Virtual Care Right for Your Dual Diagnosis Needs?
- Do you face transportation, mobility, or distance barriers to in-person care?
- Is your schedule unpredictable, making regular on-site attendance tough?
- Does your area lack specialized dual diagnosis services?
- Are you comfortable with video, phone, or secure messaging platforms?
- Would home-based support help you feel safer or more engaged?
Virtual care has become a lifeline for many seeking dual diagnosis services, especially in rural or underserved regions where finding integrated treatment on-site can be nearly impossible10. With telehealth, you can connect to licensed therapists, prescribers, and peer support via secure video or phone—sometimes even outside of standard hours.
This path makes sense for professionals who need flexibility, live far from major treatment centers, or want to continue progress during travel or life transitions. Virtual dual diagnosis services require a reliable internet connection, a private space, and basic tech skills. For example, accessing your sessions might be as simple as entering your credentials and pressing Enter to join a HIPAA-compliant video room.
For most clients, sessions last 45–60 minutes and follow a similar rhythm to in-person care, including therapy, medication management, and progress reviews. Research confirms that telehealth can be just as effective as face-to-face treatment for many co-occurring disorders, with high satisfaction rates and strong retention5. Yes, tech hiccups or privacy concerns can make things challenging, but every time you show up—virtually or not—you’re building momentum.
Your Role in Treatment Success
Active Engagement Strategies
Active Engagement Checklist: How to Boost Your Participation in Dual Diagnosis Services
- Attend all scheduled therapy and medication management sessions
- Complete homework or practice assignments between appointments
- Track your mood, cravings, or triggers in a journal or app
- Be open and honest with your treatment team, even when it’s uncomfortable
- Set small, realistic goals for each week, and celebrate progress
- Ask questions and voice concerns—your feedback shapes your care
Active participation is a strong predictor of success in dual diagnosis services. That means showing up, following through on assignments, and being honest about your challenges—especially on days when motivation is low. You’re not expected to be perfect; what counts is that you keep showing up and try again.
Every time you speak up in group, reflect on a session, or share a tough experience with your provider, you strengthen your foundation for recovery. Research shows that greater engagement directly improves outcomes and increases treatment retention for people with co-occurring disorders3. This solution fits individuals who thrive with structure and appreciate seeing their efforts pay off over time.
Remember, even small steps—like tracking your mood using a daily-tracker application or attending an extra meeting—add up. If a strategy isn’t working, let your team know so adjustments can be made. Progress isn’t always fast, but every bit of engagement moves you forward. Next, you’ll learn how building a strong support network can further improve your treatment experience.
Building Your Support Network
Support Network Builder: Who’s on Your Team?

- Trusted family members or partners
- Friends who respect your recovery goals
- Peer support groups (in-person or virtual)
- Sponsors, mentors, or recovery coaches
- Faith leaders or spiritual guides (if meaningful to you)
- Other professionals: counselors, social workers, or case managers
Building a support network within dual diagnosis services isn’t just about having people around—it’s about creating a circle that understands, encourages, and holds you up when things get tough. Recovery is rarely a solo journey. You’ll likely notice the difference when someone checks in after a hard day, joins you for a meeting, or simply listens without judgment.
Each connection can add another layer of strength, especially on days when your own confidence wavers. Research shows that family involvement and peer support both increase treatment retention and long-term success for people with co-occurring disorders7. Prioritize this when you value accountability, need encouragement, or want to reduce isolation as you work through recovery challenges.
Network Tip: Quality over quantity. One reliable supporter is better than a dozen inconsistent ones.Sometimes, you may need to set new boundaries or take a break from those who don’t support your healing—that’s okay, too. Every relationship you nurture for your recovery is a victory. Your support network isn’t fixed; it can grow and evolve as your needs change. Next, you’ll find answers to common questions about dual diagnosis services to help clarify your next steps.
Frequently Asked Questions
How do I know if I need dual diagnosis services instead of single-focus treatment?
If you’re noticing that substance use and mental health symptoms often overlap, intensify each other, or don’t improve with single-focus treatment, dual diagnosis services may be the right fit. This approach works best when addressing just one concern hasn’t led to lasting change, or if you’ve experienced repeated setbacks after single-issue care. About 50% of people with a substance use disorder also face a mental health disorder, so these patterns are more common than you might think1. Dual diagnosis services are designed for those who need coordinated support for both conditions, helping you break frustrating cycles and move forward with hope.
What happens during the initial assessment for dual diagnosis services?
During the initial assessment for dual diagnosis services, you can expect a thorough, supportive process that looks at all aspects of your health and history. This usually involves meeting with a multidisciplinary team—often a therapist, medical provider, and sometimes a peer specialist. They’ll ask about your substance use patterns, mental health symptoms, past treatments, physical health, family background, and any trauma or risk factors. The goal is not just to collect information, but to understand your strengths, challenges, and support systems. This detailed approach creates a personalized treatment plan that addresses both conditions together, setting you up for better outcomes3. Every detail you share helps build a stronger foundation for your recovery.
How long does dual diagnosis treatment typically take before I see progress?
Progress in dual diagnosis services can look different for everyone, and that’s completely normal. Many people start to notice small improvements—like better sleep, fewer cravings, or increased hope—within the first few weeks of consistent treatment. Full benefits, such as stronger coping skills and improved stability, often develop over several months. Research shows that integrated care models typically require 12–24 sessions or more to see measurable gains, depending on individual needs and level of engagement3. Remember, every step forward counts, even if it feels slow at times. Stay connected with your team and celebrate each milestone along the way.
Can I receive dual diagnosis services if I live in a rural area with limited local options?
Absolutely—you can access dual diagnosis services even if you live in a rural area with limited local resources. The rise of virtual care has made a real difference for professionals and clients outside major cities, letting you connect with licensed specialists via secure video, phone, or messaging platforms. Telehealth options help bridge the gap where in-person programs are scarce, and research shows they are just as effective as traditional face-to-face care for many with co-occurring conditions510. All you’ll need is a reliable internet connection, a private space, and basic tech skills. Remember, every effort to seek support counts—you deserve quality care, no matter your location.
What if my symptoms overlap and providers can’t tell which condition is causing what?
It’s completely normal for symptoms to blur together so much that even experienced providers can’t always pinpoint which condition is causing what. Dual diagnosis services are built with this challenge in mind—rather than forcing a clear separation, integrated care focuses on treating both mental health and substance use symptoms at the same time. This approach works best when the lines are fuzzy, since it reduces the risk of missing something important or letting one issue go untreated. Research confirms that when both conditions are addressed together, people have better outcomes and higher treatment retention3. Remember, you don’t have to have all the answers for care to work—showing up and being honest with your team is what truly matters.
Will insurance cover dual diagnosis services or do I need separate coverage for each condition?
Most insurance plans are now required to cover mental health and substance use treatment at a similar level to other medical care, thanks to mental health parity laws10. This means dual diagnosis services are often included under your primary insurance policy, so you usually don’t need separate coverage for each condition. If you’re unsure, check your policy details or reach out to your insurance representative—they can explain exactly what’s covered and if there are any pre-authorization steps. Remember, persistence pays off here—navigating insurance can be frustrating, but every question you ask brings you closer to the support you deserve.
How do I choose between different dual diagnosis programs when they all seem similar?
Choosing between dual diagnosis programs can feel overwhelming when they seem so similar on the surface. Start by comparing the structure and flexibility—some offer daily in-person sessions, while others focus on virtual care or evening hours. Look for programs that provide a truly integrated approach, with a multidisciplinary team addressing both mental health and substance use needs at the same time. Pay attention to their use of evidence-based therapies and the level of peer or family involvement offered. This approach is ideal if you value a team that communicates closely and supports your engagement throughout treatment. Research shows that programs emphasizing coordinated, whole-person care deliver stronger results and higher retention rates3. Trust your instincts—if a program feels supportive and adapts to your needs, it’s likely the right fit for your journey.
Your Path Forward Starts Here
Integrated dual diagnosis services demonstrate measurably better outcomes when they address co-occurring substance use and mental health disorders simultaneously rather than treating these conditions in isolation. Research consistently shows that individuals presenting with both substance use disorders and conditions such as anxiety, depression, PTSD, or bipolar disorder require specialized treatment protocols that acknowledge the complex interplay between these conditions.
Effective dual diagnosis services incorporate evidence-based modalities including cognitive behavioral therapy and dialectical behavioral therapy within a trauma-informed framework. These therapeutic approaches, when delivered through structured programming, provide the clinical foundation necessary for sustainable recovery. Partial hospitalization programs offer intensive therapeutic support with medical oversight, while intensive outpatient programs deliver comprehensive treatment within a flexible structure that accommodates professional responsibilities. Both modalities have demonstrated efficacy when properly implemented.
Geographic barriers to treatment continue to affect rural populations disproportionately. Virtual treatment delivery models have expanded access significantly, enabling individuals in underserved areas to receive the same evidence-based dual diagnosis services available in traditional clinical settings. This treatment modality has proven particularly valuable for professionals where provider shortages create access challenges. Virtual PHP and IOP programs address this gap while maintaining clinical rigor and therapeutic continuity.
Culturally responsive care represents another critical component of comprehensive dual diagnosis services. Programs incorporating culturally grounded healing frameworks alongside conventional therapeutic modalities demonstrate improved engagement and outcomes. This integrated approach recognizes that effective care must address identity, historical trauma, and community connection as essential elements of the recovery process, not peripheral considerations. You have the tools and the knowledge—now it’s time to take that courageous next step toward healing.
References
- Dual Diagnosis (Co-Occurring Disorders). https://my.clevelandclinic.org/health/diseases/24921-dual-diagnosis
- Substance Use Disorder and Mental Illness Often Go Hand in Hand. Both Must Be Addressed.. https://www.columbiadoctors.org/news/substance-use-disorder-and-mental-illness-often-go-hand-hand-both-must-be-addressed
- Integrated Treatment of Substance Use and Psychiatric Disorders. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3753025/
- Psychosocial interventions in patients with dual diagnosis. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5844161/
- Getting Mental Health Support Virtually. https://www.nimh.nih.gov/health/topics/telehealth
- Evidence-based practices for substance use disorders. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3678283/
- Family Involvement in Treatment and Recovery for Substance Use Disorders. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8380649/
- Stigma and Discrimination. https://nida.nih.gov/research-topics/stigma-discrimination
- The Impact of Co-occurring Post-traumatic Stress Disorder and Substance Use Disorders. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8712572/
- Treatment Access Barriers and Disparities Among Individuals with Co-occurring Disorders. https://www.ncbi.nlm.nih.gov/pmc/articles/PMC4695242/






