Key Takeaways
- Assessment Scoring Guide: Evaluate clients for both substance use and mental health symptoms simultaneously to accurately identify alcohol dual diagnosis.
- Top 3 Success Factors: 1) Integrated care models (improving retention significantly), 2) Trauma-informed environments, and 3) Consistent step-down support like Intensive Outpatient Programs (IOP).
- Immediate Next Action: Implement a standardized dual-screening protocol in your intake process to ensure no overlapping symptoms are missed.
What Alcohol Dual Diagnosis Really Means
Understanding alcohol dual diagnosis is essential for professionals dedicated to providing safe, medically supervised treatment. When you and your team encounter clients facing these overlapping challenges, it can feel overwhelming—and that is completely okay. Every step forward counts in building an effective, compassionate care plan.
The Connection Between Mental Health and Alcohol Use
Let’s start with a practical tool to guide your clinical understanding and intake process:
Quick Assessment: Are Both Alcohol Use and Mental Health Symptoms Present?
- Do you or your clients notice persistent feelings of sadness, anxiety, or mood swings along with frequent alcohol use?
- Are symptoms of depression, PTSD, or panic attacks made worse by drinking, or does drinking seem like a way to cope?
- Has increased alcohol use led to issues at work, home, or in relationships?
If you answered yes to more than one, you’re likely seeing the connection that defines alcohol dual diagnosis. This means someone is facing both a mental health condition (like depression, anxiety, or PTSD) and an alcohol use disorder at the same time. These conditions often feed into each other. For example, people experiencing depression or anxiety may use alcohol to numb emotional pain, seeking relief that’s unfortunately short-lived.
The self-medication cycle can quickly set in, trapping people in a pattern that worsens both issues over time1. The numbers highlight this strong tie:
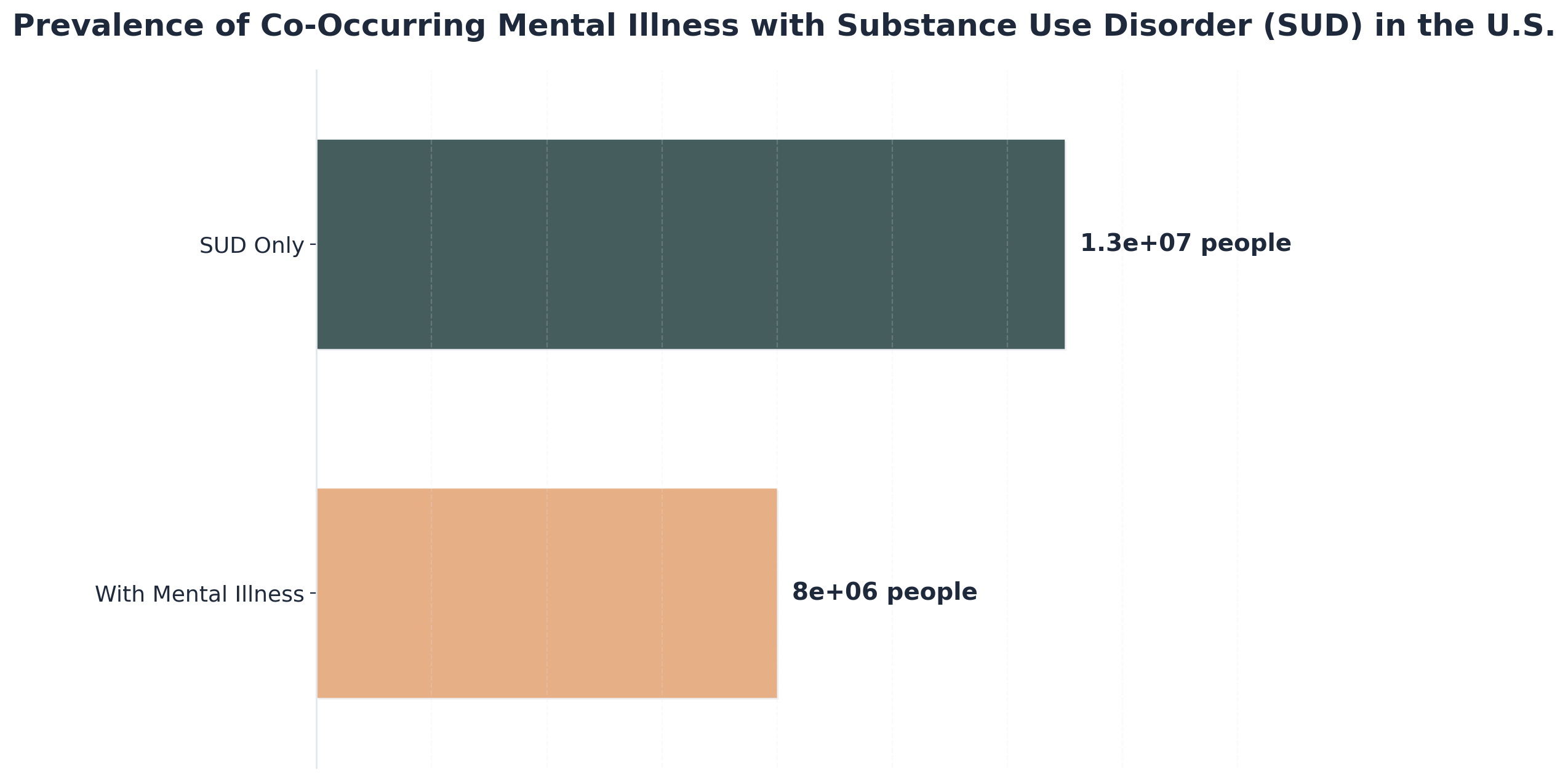
“Individuals with a mental illness consume about 38% of all alcohol in the United States, and more than twice as many people with mental health conditions struggle with substance use compared to those without.”1
Yes, this is challenging—and that’s okay. Recognizing the overlap is a powerful first step for your practice. Every step forward counts! Up next, you’ll learn how to spot when both challenges are present.
Recognizing When You’re Facing Both Challenges
To help clarify when alcohol dual diagnosis is present, use this simple screening tool during your evaluations:
- Symptom Timeline: Are symptoms of depression, anxiety, PTSD, or mood disorder noticeable before drinking starts?
- Withdrawal Impact: Does alcohol use make these symptoms worse the next day or during withdrawal?
- Coping Mechanisms: Is there a pattern of using alcohol to cope with emotional pain, trauma, or stress?
- Reduction Attempts: Have attempts to reduce drinking led to spikes in anxiety, sadness, or irritability?
If most answers are yes, there’s a strong chance both mental health and alcohol use disorders are interacting. Recognizing this overlap is hard work—it takes honesty and courage to look at the full picture. This approach works best when your clinical team needs to move beyond surface symptoms and get to the root of persistent challenges.
It’s common to see alcohol dual diagnosis missed because symptoms appear separately or are mistaken for other problems1. For example, someone may seek help for depression without mentioning drinking habits, or vice versa. This can leave the real issues untreated and prolong suffering. About half of people who experience a mental illness during their lives will also experience a substance use disorder at some point, and vice versa2.
If you are noticing both sets of symptoms in your clients, acknowledge the progress in spotting a tough pattern—every bit of clinical awareness is a win! Up next, you’ll see why these conditions tend to keep each other going.
Why Alcohol Dual Diagnosis Conditions Fuel Each Other
The Self-Medication Cycle That Keeps You Stuck
Let’s kick off with a clear visual framework for your team or clients to understand the progression of alcohol dual diagnosis:
| Stage | Client Experience | Clinical Observation |
|---|---|---|
| 1. Trigger | Mental health symptoms (like anxiety or depression) rise. | Increased distress, isolation, or agitation. |
| 2. Action | Alcohol is used for quick relief. | Self-medicating behavior to numb emotional pain. |
| 3. Rebound | Temporary numbness is followed by rebound symptoms. | Symptoms return, often worse than before. |
| 4. Reinforcement | Guilt, shame, or withdrawal adds new stress. | Fueling another round of drinking, solidifying the cycle. |
This cycle is at the core of alcohol dual diagnosis. The self-medication hypothesis explains why so many people get stuck: alcohol soothes deeply uncomfortable feelings, but only for a short time. You probably see this in practice—someone feels overwhelmed by trauma, panic, or sadness, turns to drinking to “take the edge off,” and then faces even harsher symptoms after the effects wear off.
Over time, the brain adapts, making both the cravings and mental health symptoms harder to manage1. This pattern is especially tough to break because each part of the cycle reinforces the next. Consider this method if you are working with clients who report escalating anxiety after drinking, or who describe drinking as their “only relief,” as it’s a strong signal that both issues feed each other.
Remember, breaking this cycle takes time and patience—every effort your practice makes to intervene counts! Next, we’ll explore how genetics and environment can raise the risk for alcohol dual diagnosis.
How Genetics and Environment Shape Your Risk
Let’s start with a practical tool for your clinical toolbox:

- Biological Factors: Does your client have a family history of substance use or mental health conditions?
- Historical Trauma: Did they experience early life stress, trauma, or instability?
- Current Environment: Are there ongoing environmental pressures, like chronic stress or community disconnection?
If you’re checking off multiple boxes, the chance of alcohol dual diagnosis is significantly higher. When documenting these risk factors in your Electronic Health Record (EHR), you might use specific diagnostic codes like F10.20 for alcohol dependence to ensure accurate tracking and billing.
Genetics play a major role: about 40–60% of someone’s vulnerability to substance use disorders comes from inherited factors4. That means even people who grow up with strong support can still be at risk if there’s a family history. But genes are only part of the picture—environment matters, too. Exposure to ongoing stress, trauma, or a lack of community resources can activate or worsen this risk.
This strategy suits organizations that strive to understand the whole person, not just their symptoms. For example, you might notice a pattern: a client with a parent who had depression and alcohol issues, plus childhood instability, may face more hurdles than someone without those layers. Yes, it’s complicated—progress here is about uncovering what’s beneath the surface.
Recognizing how risk factors add up gives you a more accurate, compassionate view of each individual’s journey. Next, you’ll discover how integrated treatment models can address both pieces of the alcohol dual diagnosis puzzle.
Treatment Approaches That Address Both Issues
Integrated Care Models and Evidence-Based Therapies
Start by equipping yourself with a practical decision tool to determine the right level of care:
- Are both alcohol use disorder and a mental health condition present at the same time?
- Has treating one condition alone failed to produce lasting progress?
- Are symptoms in one area (mental health or alcohol use) making the other worse?
- Is the client open to coordinated, team-based care?
When you find yourself answering yes, integrated care models may be the right fit. Integrated care means treating both substance use and mental health conditions together—using a team approach where clinicians collaborate, share information, and tailor therapies to the whole person. This method is especially effective for alcohol dual diagnosis, where treating just one issue rarely breaks the cycle for good1.
Evidence-based therapies are the backbone here. Cognitive Behavioral Therapy (CBT) helps people spot and shift negative thought patterns fueling both drinking and emotional distress. Dialectical Behavior Therapy (DBT) builds skills for emotion regulation, distress tolerance, and healthy relationships—tools that matter when both disorders are present. Group therapy and psychoeducation reinforce what’s learned in individual sessions, offering belonging and validation.
Opt for this framework when your client’s symptoms blend together or worsen in tandem. For example, if someone’s anxiety spikes during alcohol withdrawal, or their drinking intensifies when depression deepens, a unified treatment plan can break the cycle and offer hope7. At facilities like Healing Rock Recovery, integrating these therapies with culturally grounded approaches like the Wellbriety program provides a holistic foundation.
Research supports this: about two-thirds of people in dual diagnosis treatment maintain improvements in both substance use and mental health after one year8. Yes, it’s demanding—but every coordinated step is meaningful progress. Next, you’ll see how medication-assisted options and trauma-informed care can deepen recovery for alcohol dual diagnosis.
Medication-Assisted Treatment and Trauma-Informed Care
Let’s start by grounding your approach with a decision tool for advanced interventions:

- Does your client experience severe withdrawal, cravings, or repeated relapse?
- Is there a history of trauma, abuse, or significant emotional distress?
- Have traditional therapies alone failed to produce or sustain recovery?
- Is the client struggling to trust providers or engage fully in treatment?
If you’re nodding yes to several, combining medication-assisted treatment (MAT) and trauma-informed care can be a crucial next step. Medication-assisted treatment involves using FDA-approved medications alongside counseling to address both alcohol cravings and withdrawal symptoms.
These medications help stabilize the brain’s chemistry, reduce the risk of relapse, and allow clients to focus on building new habits. This approach is often well-suited for individuals whose alcohol use is deeply entrenched or who have not succeeded with talk therapy alone. Research confirms that MAT, when paired with mental health support, improves outcomes for people with alcohol dual diagnosis4.
Trauma-informed care recognizes that many experiencing alcohol dual diagnosis have lived through trauma—sometimes unspoken or unrecognized. By acknowledging trauma’s impact, you help reduce shame and avoid re-traumatization. Techniques include grounding exercises, transparent communication, and honoring personal choice.
This path makes sense for teams facing high relapse rates or client disengagement. It’s not easy work, but every bit of trust built is a foundation for lasting healing. Remember: small shifts in safety and support make a real difference—celebrate those steps! Next, you’ll explore how to build a recovery plan that sustains momentum beyond structured treatment.
Building Your Recovery Path Forward
Recovery frameworks in integrated care settings rarely follow linear progressions, and understanding this reality shapes how we design effective treatment pathways. The therapeutic journey reflects complex interactions between clinical interventions, individual resilience factors, and the support systems we help clients establish. As professionals in this field, we recognize that sustainable outcomes emerge from comprehensive approaches that honor each person’s unique presentation.
Effective treatment planning begins with thorough clinical assessment that captures both presenting challenges and available resources. This assessment informs appropriate level-of-care decisions. To help your team visualize these options, consider the following structure:
| Program Type | Time Investment | Best Suited For |
|---|---|---|
| Partial Hospitalization Program (PHP) | 5-6 days/week, 4-6 hours/day | Acute stabilization, structured daily support, and intensive dual diagnosis management. |
| Intensive Outpatient Program (IOP) | 3-5 days/week, 3 hours/day | Stepping down from PHP; balancing treatment with work or family obligations. |
Comprehensive recovery frameworks must address the full spectrum of client well-being. Dual diagnosis treatment protocols recognize that co-occurring mental health conditions and substance use disorders require simultaneous, integrated intervention rather than sequential approaches. When we address underlying conditions like anxiety, depression, or trauma alongside substance use disorders, we establish more stable foundations for sustained recovery outcomes.
Evidence-based therapeutic modalities form the backbone of effective programming. Cognitive behavioral therapy provides clients with cognitive restructuring skills and behavioral activation strategies, while dialectical behavioral therapy strengthens emotional regulation and distress tolerance capacities that support long-term stability. Trauma therapy addresses adverse experiences that often contribute to substance use patterns, creating opportunities for deeper healing that extends beyond symptom management.
Effective program design incorporates diverse therapeutic modalities that address different aspects of recovery. Creative approaches like art therapy or music therapy offer alternative processing pathways that complement traditional talk therapy. Medically assisted treatment addresses physiological components of recovery that behavioral interventions alone cannot fully resolve.
Virtual intensive outpatient programs expand access for clients managing work or family obligations. Encourage your team to utilize digital tools, pressing Enter on virtual telehealth platforms to maintain connection even from rural areas. Our professional development in these areas enhances our capacity to deliver truly personalized, comprehensive care. Collaboration and consultation strengthen our clinical practice, demonstrating our commitment to excellence in integrated care approaches that serve our clients’ healing journeys.
Frequently Asked Questions
How long does it typically take to see improvement when treating both conditions together?
When treating alcohol dual diagnosis, most professionals notice initial improvements in symptoms within a few weeks to a few months. For example, mood and anxiety symptoms may start to ease after several weeks of integrated care, while reductions in alcohol use often follow as mental health stabilizes. About two-thirds of people experience significant progress in both areas after one year of dual diagnosis treatment8. This approach works best when therapy, medication, and support systems are combined—healing is gradual, and every small step matters. Progress can be slow at times, and that’s completely normal. Celebrate each milestone, knowing that consistent effort builds long-term change.
Can virtual treatment programs be as effective as in-person care for alcohol dual diagnosis?
Virtual treatment programs can absolutely support recovery from alcohol dual diagnosis as effectively as in-person care for many individuals. Recent years have shown that integrated therapies like Cognitive Behavioral Therapy (CBT), medication-assisted treatment, and support groups are adaptable to secure telehealth formats. Digital access helps break down barriers, especially for rural professionals or those managing busy schedules. Research highlights that outcomes for virtual and in-person integrated care are often similar when the program is structured well and includes regular check-ins, group interaction, and clinical oversight11. This option fits those seeking flexibility or facing geographic or mobility challenges. Remember—progress is valid, whether you’re logging in from home or walking into a clinic. Every connection counts!
What role does family history play in developing co-occurring disorders?
Family history plays a powerful role in developing co-occurring disorders like alcohol dual diagnosis. Genetics can account for about 40–60% of a person’s vulnerability to substance use disorders, meaning if substance misuse or mental illness is present in your family tree, your risk is higher4. If you’ve noticed several generations with alcohol problems, depression, or anxiety, it’s not your fault—these patterns often begin with inherited biology. That said, genes aren’t destiny. A tough family history doesn’t guarantee you’ll face both challenges, but it does mean extra support and early intervention are key. Recognize your resilience in seeking answers and know that change is possible, even with a complicated background.
How do I know if I need a partial hospitalization program versus an outpatient program?
Choosing between a partial hospitalization program (PHP) and an outpatient program often depends on the intensity of your symptoms and daily support needs. PHP is usually a good fit if you or your client need structured care most of the day, especially when safety, stability, or withdrawal management are top concerns. Outpatient programs work well when symptoms are more stable and daily life can be managed with less intensive support. This distinction matters in alcohol dual diagnosis, where co-occurring mental health and substance use symptoms can change rapidly4. If frequent crises, severe withdrawal, or limited home support are present, PHP may provide the extra structure needed. Remember, asking for more help is a sign of strength, not failure.
What happens if my mental health symptoms get worse during alcohol withdrawal?
Worsening mental health symptoms—like anxiety, depression, or panic—during alcohol withdrawal is common in alcohol dual diagnosis cases. This spike happens because alcohol affects brain chemicals that help regulate mood; when use stops, the brain needs time to adjust4. You might see clients experience intense mood swings, agitation, or even suicidal thoughts during early withdrawal. This is challenging, and it’s not a sign of failure. Prioritize close monitoring and rapid access to medical and therapeutic support in these moments. Integrated care teams can help stabilize symptoms safely, offering reassurance and a sense of safety through the toughest days. Every bit of support during withdrawal is a victory—progress is possible.
Are there specific therapies that work better for certain mental health and alcohol combinations?
Certain therapies are a better fit for specific alcohol dual diagnosis combinations. For instance, Cognitive Behavioral Therapy (CBT) is especially effective for depression or anxiety alongside alcohol use, helping clients reframe negative thoughts and develop coping skills4. Dialectical Behavior Therapy (DBT) offers strong results when emotional regulation is a challenge, such as with borderline personality or bipolar disorder. Trauma-focused therapies—including EMDR and trauma-informed CBT—are often most helpful when PTSD is present with alcohol use issues4. This approach works best when you match therapy to both the mental health diagnosis and each person’s strengths. Remember, every tailored intervention brings hope—celebrate those moments of improvement, no matter how small.
How can I maintain progress after completing a structured treatment program?
Maintaining progress after a structured treatment program for alcohol dual diagnosis calls for a thoughtful, ongoing plan. Encourage regular check-ins—therapy sessions, peer support, or virtual appointments all reinforce recovery. Help clients identify early warning signs of stress, cravings, or mood dips, and rehearse simple coping strategies together. Building a daily routine with healthy sleep, nutrition, and meaningful activities creates stability. This solution fits professionals supporting clients who need flexibility, as digital tools and telehealth can extend care beyond the clinic. Research shows that those with consistent follow-up and community support have better outcomes, with two-thirds maintaining gains after one year8. Every bit of continued effort matters—progress is always worth celebrating.
Your Next Steps Toward Healing
Implementing effective alcohol dual diagnosis treatment requires a comprehensive framework that addresses both substance use and mental health needs simultaneously. As you develop or refine your integrated care approach, consider how these evidence-based practices can strengthen treatment outcomes in your setting.
// Example Intake Protocol Flow
1. Initial Screening (PHQ-9, GAD-7, AUDIT)
2. Dual Diagnosis Flagging
3. Integrated Psychiatric & Clinical Assessment
4. Level of Care Determination (PHP/IOP)
Successful dual diagnosis treatment depends on coordinated assessment protocols that identify co-occurring conditions early in the treatment process. Your clinical team’s ability to recognize the interconnected nature of substance use disorders and mental health challenges directly impacts treatment planning effectiveness. Consider how your current intake procedures support comprehensive dual diagnosis evaluation and whether your staff training adequately prepares clinicians for integrated care delivery.
The therapeutic modalities discussed throughout this framework—including cognitive behavioral therapy, dialectical behavioral therapy, trauma-informed approaches, and culturally responsive interventions—work most effectively when delivered within a cohesive treatment structure. Whether you’re implementing partial hospitalization programs, intensive outpatient treatment, or hybrid models, maintaining fidelity to dual diagnosis treatment principles ensures that neither condition receives inadequate attention.
“Your ongoing professional development in dual diagnosis treatment methodologies ultimately translates to improved patient outcomes and more sustainable recovery trajectories for those you serve.”
As the field continues advancing, staying current with emerging alcohol dual diagnosis research, attending specialized training opportunities, and collaborating with peers who share your commitment to integrated care will strengthen your clinical expertise. This solution fits professionals who are dedicated to continuous improvement and compassionate care.
References
- NAMI. Understanding Dual Diagnosis.. https://www.nami.org/Blogs/NAMI-Blog/October-2017/Understanding-Dual-Diagnosis
- NCBI/NIH. Common Comorbidities with Substance Use Disorders.. https://www.ncbi.nlm.nih.gov/books/NBK571451/
- NCBI/PMC. The Epidemiology of Post-Traumatic Stress Disorder and Alcohol Use Disorder.. https://pmc.ncbi.nlm.nih.gov/articles/PMC6561398/
- NCBI/PMC. Anxiety and Alcohol Use Disorders: Comorbidity and Treatment.. https://pmc.ncbi.nlm.nih.gov/articles/PMC3860396/
- NCBI/PMC. Bipolar Disorder and Alcoholism.. https://pmc.ncbi.nlm.nih.gov/articles/PMC6683827/
- SAMHSA. Managing Life with Co-Occurring Disorders.. https://www.samhsa.gov/mental-health/serious-mental-illness/co-occurring-disorders
- NIAAA. Recommend Evidence-Based Treatment: Know the Options.. https://www.niaaa.nih.gov/health-professionals-communities/core-resource-on-alcohol/recommend-evidence-based-treatment-know-options
- NCBI/PMC. The Effects of Residential Dual Diagnosis Treatment on Alcohol Abuse.. https://pmc.ncbi.nlm.nih.gov/articles/PMC5576155/
- NCBI/PMC. Belief, Behavior, and Belonging: How Faith is Indispensable to Addiction Recovery.. https://pmc.ncbi.nlm.nih.gov/articles/PMC6759672/
- Yale Medicine. How an Addicted Brain Works.. https://www.yalemedicine.org/news/how-an-addicted-brain-works






