Key Takeaways: Your Recovery Roadmap
- Assess Your Needs: Determine if you require the structure of a daily clinic (Methadone) or the flexibility of an office-based prescription (Buprenorphine).
- Understand the Science: Medication-assisted treatment reduces the risk of overdose death by approximately 50% compared to behavioral therapy alone.
- Integrate Care: The most effective plans combine FDA-approved medication with counseling to address both physical cravings and emotional health.
- Take Action: Check your insurance for “prior authorization” requirements and ask a provider about telehealth options if you are in a rural area.
What Medication-Assisted Treatment Really Means
How MAT Combines Medication and Support
Let’s break down how medication-assisted treatment weaves together the power of medication with the support you need for real, lasting recovery. This approach uses FDA-approved medications to help reduce cravings and withdrawal symptoms, making it easier for you to focus on healing. However, the real strength comes from combining medication with therapy, counseling, and community support.
Here’s a simple checklist to help you understand what’s usually included in a well-rounded medication-assisted treatment plan:
- Medication management and regular check-ins with a provider.
- Individual or group therapy sessions.
- Peer support or recovery coaching.
- Family involvement, when possible.
- Ongoing education about wellness and relapse prevention.
This approach is ideal for people who want more than just a prescription. If you’re looking for deeper change—not just physical relief—combining medication with counseling and social support is shown to help people stay in treatment and avoid relapse. In fact, the most recent evidence suggests that integrating psychosocial supports with medication can improve engagement, address mental health needs, and support long-term success6.
Consider this route if you want a recovery plan that recognizes the challenges you face and surrounds you with a compassionate team. Every step you take, from attending therapy to connecting with others, builds a stronger foundation for recovery.
The Science Behind MAT Effectiveness
Let’s take a closer look at why medication-assisted treatment is so effective—and how it’s grounded in solid science. Research shows that using medications like methadone and buprenorphine alongside supportive care leads to dramatically better outcomes than using talk therapy or medications alone.
“People who participate in medication-assisted treatment have about a 50% lower risk of dying from opioid use disorder compared to those who go without this kind of support.” 4
This isn’t just about numbers—medication-assisted treatment works by targeting both your body and your mind. Medications stabilize brain chemistry, ease withdrawal, and quiet cravings so you can focus on rebuilding your life. At the same time, counseling and connection help you heal emotionally and prepare for long-term success. When these elements come together, you get a treatment approach that’s been proven to keep people in recovery programs longer and reduce the risk of returning to use1.
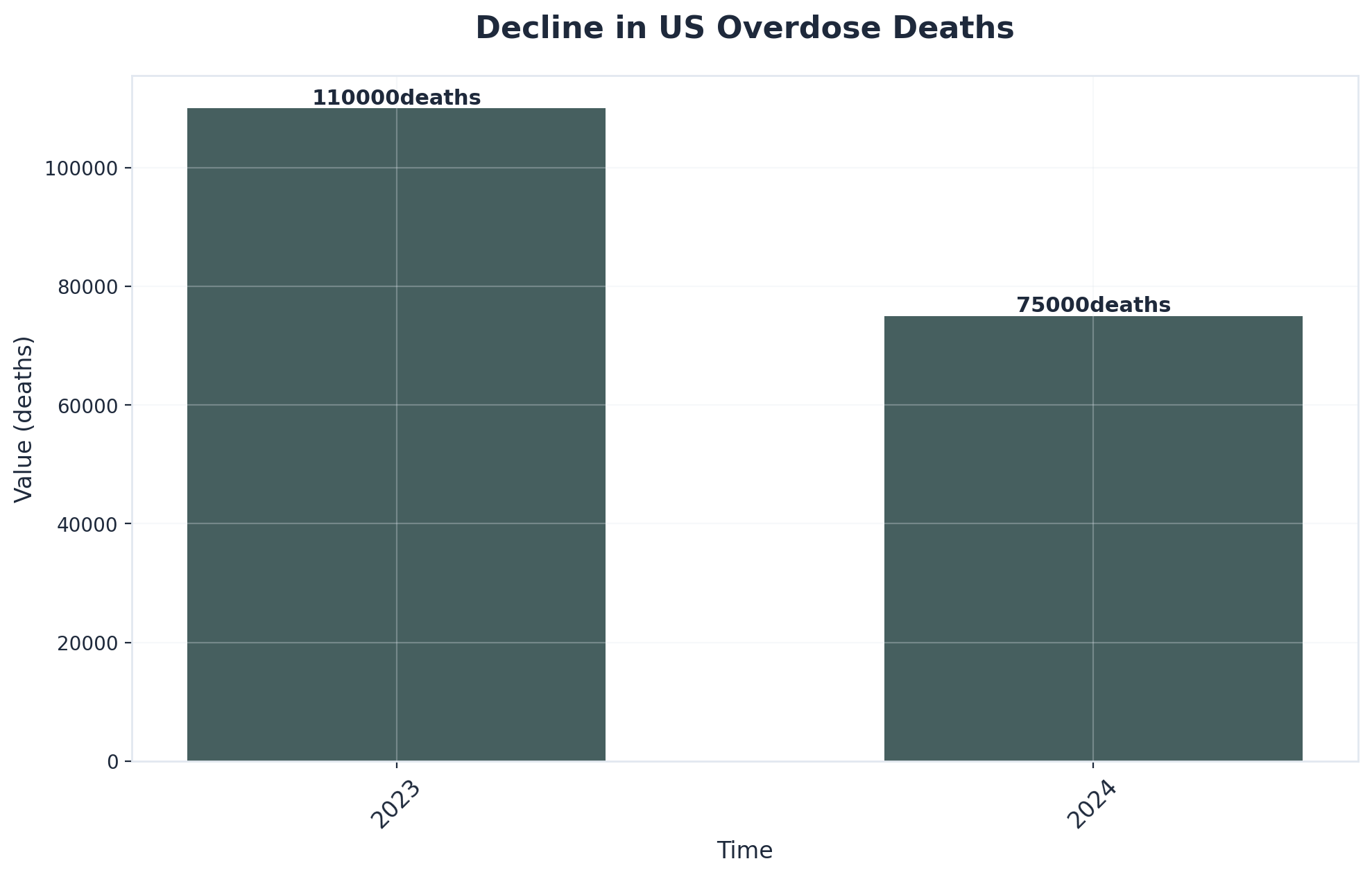
Recent progress in medication-assisted treatment is helping save even more lives. For example, overdose deaths in the U.S. fell sharply from over 110,000 in 2023 to about 75,000 in 2024, a change attributed in part to better access to these treatments3. Knowing the science can give you real hope: recovery isn’t just possible—it’s something you can build step by step.
FDA-Approved Medications and How They Work
Methadone and Buprenorphine for Stability
If you’re exploring your options for medication-assisted treatment, methadone and buprenorphine are two of the most widely used medications for building stability in recovery. Both are FDA-approved and work by easing withdrawal symptoms, reducing cravings, and helping you regain balance in your daily life.
| Feature | Methadone | Buprenorphine |
|---|---|---|
| Type | Full Agonist (Fully activates receptors) | Partial Agonist (Partially activates receptors) |
| Access | Specialized Clinics (OTP) | Doctor’s Office, Clinic, or Telehealth |
| Best For | People needing daily structure and supervision | People needing flexibility and lower overdose risk |
Methadone is known as a full agonist, which means it fully activates the opioid receptors in your brain, but in a controlled way. This helps stop the cycle of highs and lows from other opioids, providing a steady foundation as you work through recovery. Methadone is usually taken once a day at a specialized clinic, and its long-acting effects mean you won’t have to worry about sudden cravings or withdrawal throughout the day. People who use methadone in medication-assisted treatment often report better retention in their programs and higher satisfaction compared to some other options3.
Buprenorphine is a partial agonist, so it activates those same receptors but to a lesser degree. This lowers your risk of overdose and allows more flexibility, as buprenorphine can be prescribed in a doctor’s office or even through telehealth. In recent years, access to buprenorphine has expanded dramatically—prescriptions increased by 83% over the last decade, partly due to new laws allowing more providers to prescribe it2.
Naltrexone and Extended-Release Options
If you’re interested in options beyond methadone and buprenorphine, naltrexone and extended-release medications may offer a different path in medication-assisted treatment. Naltrexone works as an opioid antagonist, meaning it blocks opioid receptors in your brain so that using opioids won’t produce any effects. This can empower you to take back control, especially if you’re committed to maintaining abstinence after detox.
Extended-release naltrexone is available as a monthly injection, making it easier to stick with your plan without daily dosing. This route is a good fit if you want a non-opioid option or if you’ve completed detox and want a treatment that doesn’t come with the risk of physical dependence. Extended-release versions can also be helpful if you find it difficult to remember daily medications or prefer less frequent appointments. While naltrexone can be highly effective, it does require that you be fully free of opioids before starting, which can be a tough step for some people3.
Integrating Therapy with Medication
When you engage in medication-assisted treatment, the medication stabilizes your physical state, but therapy provides the tools to rebuild your life. You don’t have to choose between the two; they are designed to work together. While medication quiets the physical noise of addiction, therapy helps you understand the “why” behind your use and equips you with strategies to handle stress, triggers, and relationships.
Research consistently shows that combining behavioral therapy with medication produces better outcomes than either treatment alone. This dual approach creates a powerful synergy: the medication allows your brain to heal enough to engage in therapy, and therapy teaches you the skills to maintain the stability the medication provides. Your treatment team plays a crucial role in coordinating this, ensuring your medical provider and counselor are aligned on your goals.
Types of Therapy That Work Well with MAT
Several evidence-based therapy approaches complement medication-assisted treatment effectively:
- Cognitive Behavioral Therapy (CBT): This helps you identify and change negative thought patterns that fuel substance use. It teaches practical skills for managing cravings and avoiding high-risk situations.
- Contingency Management: This approach uses positive reinforcement, such as vouchers or rewards, to encourage healthy behaviors like attending appointments and staying substance-free.
- Family Therapy: Addiction affects the whole family. This therapy helps repair relationships and builds a supportive home environment, which is critical for long-term recovery.
Overcoming Barriers to Integrated Care
Accessing both medication and therapy can sometimes present challenges. Cost is often a primary concern, as you are paying for two types of service. If you have insurance, check your benefits carefully—many plans cover both services under medication-assisted treatment guidelines. Finding providers who communicate effectively with each other is also key. You can facilitate this by signing release forms that allow your doctor and therapist to share information.
How to Get Started with Combined Treatment
Taking the first step toward integrated medication-assisted treatment begins with asking your current provider about comprehensive care. If you are at a clinic for methadone, ask about their counseling requirements. If you are seeing a doctor for buprenorphine, ask for a referral to a therapist who specializes in addiction. Be prepared to advocate for yourself; you deserve a care plan that treats the whole person, not just the symptoms.
Overcoming Barriers to MAT Access
Addressing Stigma and Misconceptions
Facing stigma can feel like another hurdle in your recovery journey, especially when it comes to medication-assisted treatment. People may hold outdated beliefs or misunderstandings, such as thinking that using medication is simply replacing one substance for another. These misconceptions can make it harder to reach out for support or stick with your plan.
Here’s a quick checklist for challenging stigma around medication-assisted treatment:
- Remember: Using medication for recovery is a medical decision, not a sign of weakness.
- Share evidence:
MATcuts the risk of dying from opioid use disorder by about 50%4. - Connect: Find others who understand your path—peer support can help break down shame and build confidence.
- Take pride: Every step you take is backed by research and recommended by medical experts.
Stigma doesn’t just come from outside; sometimes, it’s internal. Remind yourself that choosing medication-assisted treatment is an act of strength and self-care. The more you learn and share about how MAT works, the more you help shift attitudes in your community.
Navigating Insurance and Policy Changes
Navigating insurance and policy changes can feel overwhelming, but getting the right support makes a huge difference on your recovery journey. Here’s a quick checklist to help you manage the practical side of accessing medication-assisted treatment:
- Check your plan: Find out if your insurance covers the medications and therapies included in medication-assisted treatment.
- Ask about prior authorization: About 50% of Medicaid enrollees still face prior authorization requirements, which can delay care at a critical time8.
- Know your state’s laws: As of 2023, 22 states have passed laws that limit or eliminate prior authorization for medications for opioid use disorder, though the details can vary a lot from state to state7.
- Use available help: Many providers and advocacy groups will help you work through paperwork, appeals, or denials if you hit a snag.
Policy changes like the removal of the federal X-waiver now make it easier for more people to get medication-assisted treatment, but insurance rules can still present hurdles5. Don’t get discouraged—every step you take to understand your coverage brings you closer to effective care.
Frequently Asked Questions
How long will I need to stay on medication-assisted treatment?
There’s no single timeline for how long someone should stay on medication-assisted treatment—it’s truly unique to each person’s needs and goals. Some people benefit from medication-assisted treatment for several months, while others may choose ongoing support for years. Research shows that longer treatment often leads to better results, including a 50% lower risk of dying from opioid use disorder compared to those who stop early 4. Your care team will help you regularly review your progress and adjust your plan, supporting you every step of the way. Remember, you can celebrate each milestone, knowing your journey is valid.
Can I access medication-assisted treatment through telehealth if I live in a rural area?
Yes, you can access medication-assisted treatment through telehealth—even if you live in a rural area. Thanks to recent policy changes, many providers now offer virtual appointments for both medication management and counseling. This makes it much easier to get support without long drives or limited local options. In fact, telehealth availability for substance use disorder treatment facilities increased by 143% between January 2020 and January 2021, opening new doors for people in remote regions 29. You’ll usually need a stable internet connection and a device for video calls. Reach out to your provider or local clinic—they can guide you step by step. Remember, help is closer than you think.
Will my insurance require prior authorization before covering medication-assisted treatment?
Your insurance may require prior authorization before covering medication-assisted treatment, depending on your plan and where you live. About half of all Medicaid beneficiaries—despite coverage mandates—still face prior authorization requirements for these medications, which can delay care at a critical time 8. The good news is that as of 2023, 22 states have passed laws that limit or eliminate prior authorization for medications for opioid use disorder, but these protections can vary 7. If you run into this hurdle, ask your provider or a patient advocate for help with the paperwork. Remember, you’re not alone—many people face this step on their recovery journey.
How do I choose between methadone, buprenorphine, and naltrexone for my recovery?
Choosing between methadone, buprenorphine, and naltrexone in medication-assisted treatment depends on your health, personal goals, and daily routine. Methadone is often best if you need daily structure and prefer in-person clinic support. Buprenorphine offers flexibility—it’s available in clinics, doctors’ offices, and sometimes through telehealth, and it carries a lower risk of overdose. Naltrexone, a non-opioid option, works well if you’ve already completed detox and want a monthly injection instead of daily medication. Research shows all three medications are effective, with methadone and buprenorphine reducing overdose risk by about 50% 3. Talk with your care team to find the right fit for your journey.
Are there medication-assisted treatment programs that incorporate cultural practices for Indigenous communities?
Yes, some medication-assisted treatment programs are designed to honor and incorporate cultural practices for Indigenous communities. For example, approaches like Wellbriety weave together traditional healing methods, such as talking circles, ceremony, and connection to elders, alongside evidence-based medical care. These programs recognize that healing is not just physical, but also spiritual and communal. If you identify as Indigenous or want care that respects your culture, ask your provider about options that blend medication-assisted treatment with culturally relevant supports. Research shows that integrating cultural practices can increase engagement and long-term recovery success for Indigenous people seeking help 1.
What happens if I need to transition from residential treatment to outpatient medication-assisted treatment?
If you’re moving from a residential program to outpatient medication-assisted treatment, you aren’t starting over—you’re building on the progress you’ve already made. This transition usually involves working closely with your care team to create a step-by-step plan. They’ll help coordinate your medication management, set up therapy or counseling appointments, and connect you with community resources. Consistency is key: regular check-ins and ongoing support help you stay focused and confident. Research shows that continuing medication-assisted treatment after leaving residential care greatly reduces the risk of relapse and supports long-term recovery 1. Remember, each step forward is a win, and your care team is there to walk beside you.
Can medication-assisted treatment help if I have both opioid use disorder and a mental health condition?
Yes, medication-assisted treatment can absolutely help if you’re facing both opioid use disorder and a mental health condition. This approach combines FDA-approved medications with therapy and counseling, which means your care team can address both your substance use and mental health needs together. Integrating support like this has been shown to improve engagement, reduce relapse, and help manage symptoms of depression, anxiety, or trauma that often go hand-in-hand with opioid use disorder 6. You deserve a care plan that sees the whole you—not just one part. Remember, reaching out for help is a strong and positive step.
Conclusion
As you consider the long-term commitment to your health, remember that building sustainable wellness often means bringing together multiple forms of support. Managing opioid use disorder effectively requires a comprehensive approach that addresses both the biological and psychological aspects of this condition. The research is clear: medication-assisted treatment—combining therapy and medication—consistently produces better outcomes than relying on a single approach alone.
Finding the right treatment is a personal journey, and what works best often evolves over time. If you are currently taking medication but not experiencing the stability you hoped for, adding therapy can help you develop coping strategies and address underlying patterns. Similarly, if therapy hasn’t provided sufficient relief from cravings, discussing medication options with your healthcare provider could provide the biological support needed to make therapeutic work more effective.
You don’t have to navigate this journey alone. Schedule an appointment with your healthcare provider or a local clinic to discuss how medication-assisted treatment can fit into your life. Working closely with professionals who understand your unique situation will help you develop a personalized approach that addresses your specific needs. With the right combination of support and evidence-based treatment, you can move toward not just managing your condition, but truly thriving.
References
- Medication-Assisted Treatment Improves Outcomes for Patients With Opioid Use Disorder. https://www.pew.org/en/research-and-analysis/fact-sheets/2016/11/medication-assisted-treatment-improves-outcomes-for-patients-with-opioid-use-disorder
- AMA 2025 Report on Substance Use and Treatment. https://www.ama-assn.org/press-center/ama-press-releases/ama-2025-report-substance-use-and-treatment
- The Effectiveness of Medication-Based Treatment for Opioid Use Disorder. https://www.ncbi.nlm.nih.gov/books/NBK541393/
- X-Waiver No Longer Required to Treat Opioid Use Disorder. https://www.acep.org/news/acep-newsroom-articles/x-waiver-no-longer-required-to-treat-opioid-use-disorder
- Waiver Elimination (MAT Act). https://www.samhsa.gov/substance-use/treatment/resources/mat-act
- Psychosocial Supports in Medication-Assisted Treatment. https://aspe.hhs.gov/reports/psychosocial-supports-medication-assisted-treatment-recent-evidence-current-practice-0
- State Laws Prohibiting Prior Authorization for Medications for Opioid Use Disorder. https://pmc.ncbi.nlm.nih.gov/articles/PMC12721913/
- Coverage and Prior Authorization Policies for Medications for Opioid Use Disorder in Medicaid. https://jamanetwork.com/journals/jama-health-forum/fullarticle/2798039
- Understanding the Opioid Overdose Epidemic – CDC. https://www.cdc.gov/overdose-prevention/about/understanding-the-opioid-overdose-epidemic.html
- Barriers to Broader Use of Medications to Treat Opioid Use Disorder. https://www.ncbi.nlm.nih.gov/books/NBK541389/








