Key Takeaways for Professional Practice
- Assess Readiness Accurately: Utilize stage-matched protocols to determine if a client is in the cycle of change in addiction or precontemplation.
- Plan for Recurrence: Normalize “recycling” through stages as a learning opportunity rather than a clinical failure.
- Integrate Care: Combine evidence-based therapies (CBT/DBT) with holistic approaches like Wellbriety for dual diagnosis efficacy.
- Sustain Momentum: Shift resource allocation from crisis management to resilience-building routines during the maintenance phase.
Understanding the Cycle of Change in Addiction
How the Five-Stage Framework Works
Let’s break down the five-stage framework that shapes the cycle of change in addiction. This model recognizes that change is rarely a straight line. Instead, it describes recovery as a series of stages: Precontemplation, Contemplation, Preparation, Action, and Maintenance.
Here’s a quick tool—a stage identification checklist:
- Precontemplation: You notice no intention to change. There’s denial or lack of awareness.
- Contemplation: You start weighing pros and cons. Ambivalence is high.
- Preparation: You make specific plans, even simple ones, to move forward.
- Action: You’re actively changing behaviors, often with professional support. This stage requires the most energy and can feel overwhelming at times.
- Maintenance: You’re focused on sustaining gains and preventing relapse. The work shifts to building routines and resilience.
Each stage comes with its own emotional hurdles and resource needs. The action stage, for example, often requires daily time commitments for therapy or peer support, and may ask you to invest several hours per week in appointments, group sessions, or self-care routines. This strategy suits organizations that want to meet people where they are, rather than expecting immediate transformation. Research shows that progressing from one stage to the next—even within a single month—can double the odds of taking meaningful action within six months.4
As you move forward, understanding why matching interventions to a person’s current stage truly matters will help you support recovery more effectively.
Why Stage-Matched Treatment Matters
Here’s a quick assessment tool: Are your interventions clearly tailored to each person’s readiness for change? If not, you may be missing a crucial step. Matching treatment strategies to someone’s current stage in the cycle of change in addiction isn’t just a best practice—it’s foundational for building motivation, trust, and long-term engagement. When you use stage-matched approaches, you help individuals feel seen and understood, reducing shame and resistance. This method works best when you’re supporting people who may cycle back and forth between stages or who struggle with ambivalence, because it meets them where they are instead of pushing them too far, too fast.

| Stage | Primary Clinical Goal | Recommended Intervention |
|---|---|---|
| Precontemplation | Build Trust & Awareness | Motivational Interviewing, Harm Reduction |
| Preparation | Develop Concrete Plans | Goal Setting, Resource Identification |
| Action | Skill Building & Behavior Change | CBT, DBT, Medically Assisted Treatment |
“Individuals who progress from one stage to the next—even in a single month—are twice as likely to take meaningful action within six months, compared to those who remain stuck in the same stage.”4
That’s a real win, not just for the person in recovery, but for the entire treatment team. Stage-matched interventions also allow you to allocate resources more efficiently. For example, those in the preparation or action stages may need more intensive therapy hours, while those in contemplation benefit most from motivational interviewing or psychoeducational groups.
As you move into the next section, we’ll look at how to identify denial and resistance in the earliest stage of this process.
Early Recognition: Precontemplation Stage
Identifying Denial and Resistance
Spotting denial and resistance in the precontemplation stage takes both empathy and a sharp eye for subtle cues. Here’s a practical recognition tool to guide your team:
Precontemplation Stage Quick-Check:
- Does the person reject feedback or minimize concerns about substance use?
- Are there frequent statements like, “I don’t have a problem,” or, “Others are overreacting”?
- Is there a pattern of avoiding conversations about change or shifting blame?
- Does the individual seem unaware of negative consequences, or attribute them to bad luck rather than substance use?
In this earliest stage of the cycle of change in addiction, people often aren’t ready to talk about change—sometimes because shame or fear feels overwhelming, not because they lack intelligence or willpower. This approach is ideal for professionals working with clients who may appear disengaged or defensive. Recognizing these signs early means you can respond with patience, not pressure, and avoid triggering more resistance.
Research shows that individuals who stay in precontemplation are far less likely to take action within six months compared to those who progress even one stage forward, highlighting how valuable early recognition can be.4 Every instance you notice and validate resistance is a chance to build trust and gently invite new awareness.
Next, let’s explore concrete clinical strategies for supporting people who are just beginning to consider change.
Clinical Approaches for This Stage
When someone is in the precontemplation stage of the cycle of change in addiction, your clinical toolbox needs a gentle, non-confrontational approach. Here’s a practical engagement tool to consider:
Precontemplation Clinical Support Checklist:
- Use open-ended questions to invite self-reflection, not debate.
- Offer affirmations that validate strengths, even if progress feels far away.
- Share neutral, factual feedback about observed behaviors without judgment.
- Respect the person’s autonomy—avoid ultimatums or scare tactics.
- Keep interventions brief and focused on building trust, not pushing for immediate change.
This path makes sense for professionals supporting individuals who aren’t yet ready to acknowledge a problem. Motivational interviewing is especially effective here, because it encourages self-exploration while lowering defensiveness.5 Small wins—like showing up, expressing any curiosity, or simply agreeing to a second conversation—deserve celebration. These moments are building blocks for future readiness.
Time investment at this stage is often minimal, with short check-ins or supportive contacts proving more effective than lengthy sessions. Resource requirements focus on staff training in motivational interviewing and trauma-informed care, as these skills reduce resistance and nurture engagement.
Research consistently shows that meeting people where they are, rather than rushing them, can double the odds of moving forward in the next stage of the cycle of change in addiction.4
Next, you’ll learn how to help individuals in the contemplation stage move past ambivalence and take meaningful first steps.
Building Momentum Through Middle Stages
Contemplation: Moving Past Ambivalence
Here’s a practical tool to use in the contemplation stage: The Ambivalence Mapping Worksheet. Invite individuals to list their reasons for and against change on paper or a whiteboard. This isn’t about persuasion—it’s about giving ambivalence a safe space, so both sides of the struggle feel seen and respected.
In the contemplation stage of the cycle of change in addiction, you’ll notice people expressing a mix of hope and hesitation. They might say, “I know things need to change, but I’m not sure I’m ready.” This is the time to lean into motivational interviewing and reflective listening. Consider this route if your team works with individuals who have started to acknowledge the costs of substance use yet remain unsure whether change is possible or worth it. Your role is to nurture self-efficacy without rushing. Small wins—such as expressing curiosity about treatment or attending an informational group—are powerful progress markers worth celebrating.
Research demonstrates that moving from contemplation to preparation within a month nearly doubles the chance of taking action within six months.4 Time investment here is moderate: expect several focused sessions or group meetings, plus space for quiet reflection. Resources should include motivational interviewing training, worksheets, and peer-led groups to reinforce hope and normalize mixed feelings.
As individuals clarify their values and build confidence, you’ll see momentum grow—setting the stage for concrete planning in the next phase.
Preparation: Creating Concrete Plans
Preparation means turning intention into action, and this stage of the cycle of change in addiction calls for practical, step-by-step planning. Here’s a simple tool to structure this phase: The Action Planning Worksheet. Use it with individuals to outline specific goals, potential obstacles, support systems, and a timeline for starting new behaviors. Encourage participants to write down their own reasons for change and personal warning signs that signal risk, not just generic answers. This makes the plan feel real and builds ownership.

In the preparation stage, people are often ready to experiment with small changes—perhaps scheduling an assessment, exploring a therapy group, or setting a quit date. This approach works best when individuals feel both hopeful and anxious about “what comes next.” Your role is to celebrate these moments of commitment, however modest, and to validate the courage it takes to move forward.
Time investment in this stage is moderate. You’ll likely spend several sessions collaboratively building the plan, discussing triggers, and developing coping strategies. Resources should include worksheets, relapse prevention tools, and access to peer support. Research shows that people who move from preparation to action within the first month are twice as likely to achieve meaningful change at six months, compared to those who stay stuck in planning mode.4
As you finish preparation, you’re ready to support individuals through the high-energy, high-risk action stage—where real-life change unfolds.
Action and Maintenance in the Cycle of Change in Addiction
The Action Stage’s High-Risk Period
The action stage is where recovery gets real—and, not surprisingly, where risk is at its highest. Here’s a practical tool for this stage: the High-Risk Trigger Planning Sheet. Use it to help individuals and teams identify specific situations, emotions, or people that could spark cravings or old habits. Encourage your team to map out coping responses ahead of time, so when stress hits, there’s a ready-made plan to follow.
During the action stage of the cycle of change in addiction, people are making daily choices to stop substance use, attend therapy, and often restructure their environments. This phase is intense: most individuals need frequent check-ins, ongoing medical or therapeutic support, and encouragement to keep going when motivation dips. Relapse risk is highest here, which makes your support vital. This solution fits organizations with the resources for high-touch contact—think daily or near-daily sessions, quick response to setbacks, and robust peer or group support options. Time investment is substantial, and staff may need to coordinate care across medical, behavioral, and social domains.
Research confirms that the action stage demands the most energy, focus, and support—yet it’s also the point where individuals gain the most confidence in their ability to change.6, 7 Yes, this is challenging, and that’s okay. Every day someone shows up, attends a group, or uses a coping skill is a step worth celebrating!
Next, we’ll explore how to help people maintain their gains and build true resilience in the maintenance stage.
Long-Term Maintenance Strategies
Long-term maintenance in the cycle of change in addiction is about building resilience, not perfection. Here’s a practical tool for this stage: the Relapse Response Plan. Work with each person to outline what to do if cravings return or setbacks happen—who to contact, which coping skills to use, how to re-engage with support, and ways to practice self-compassion. This plan makes it much easier to bounce back quickly and avoids shame spirals that can undo months of progress.
At this point, you’ll notice the focus shifts from daily crisis management to creating sustainable routines—routine sleep, nutrition, physical activity, and ongoing peer support. Peer mentorship, alumni groups, and regular check-ins become especially valuable. This method works when your organization can offer flexible, lower-intensity supports like weekly groups, monthly alumni events, or virtual touchpoints. Time investment is lower than in the action stage, but consistency matters—encourage teams to celebrate anniversaries, skill milestones, and even healthy responses to slips.
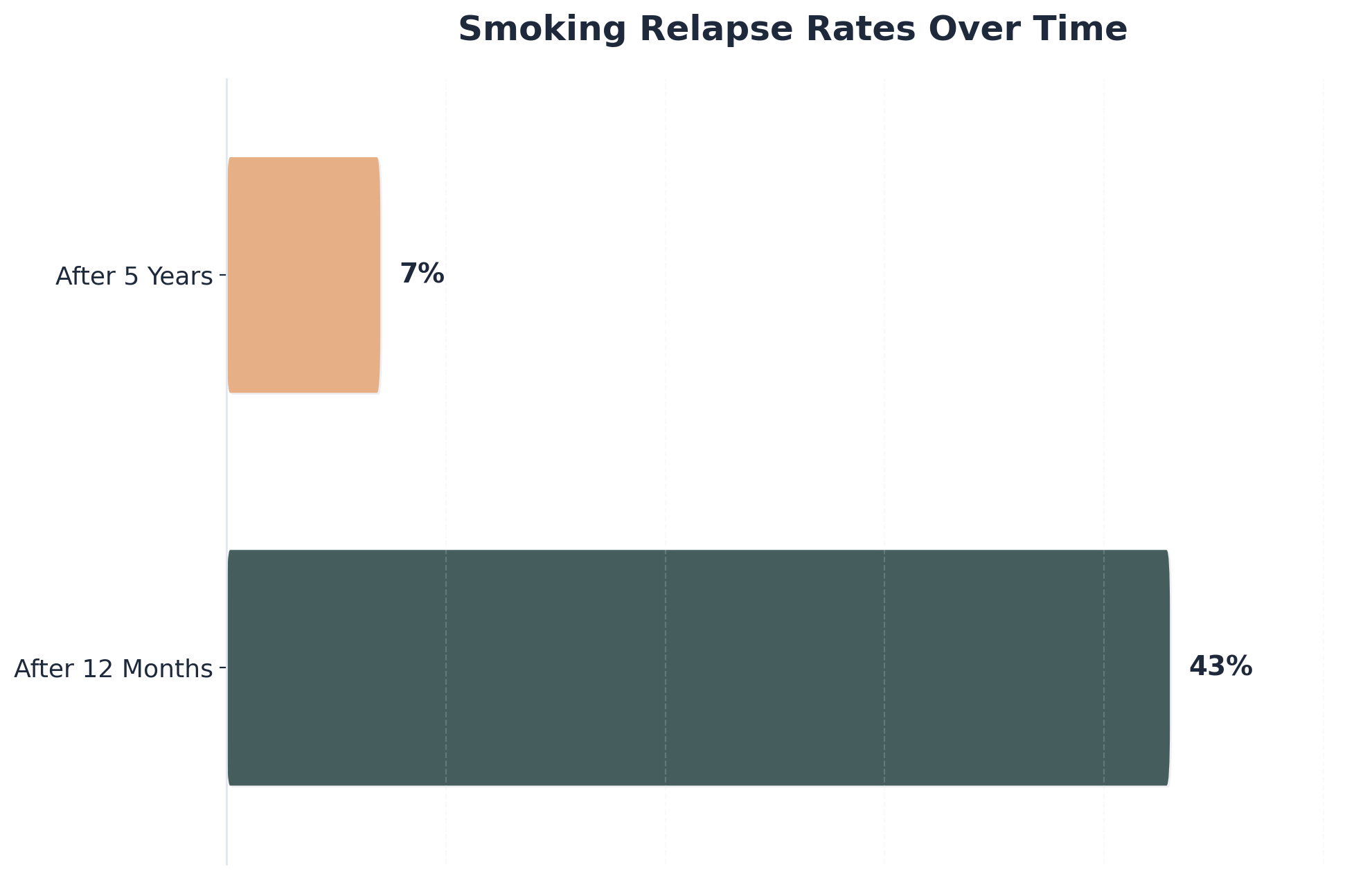
“Research highlights that relapse rates drop dramatically over time: 43% of people abstinent for one year relapse, but after five years, the rate drops to just 7%.”4
Relapse is not a failure—it’s part of the process for many. When you frame maintenance as an ongoing opportunity for growth, you help individuals stay hopeful and engaged. Every year someone maintains progress is a victory worth honoring!
As you continue, you’ll find that addressing common questions about setbacks and progress keeps your team and your clients moving forward with confidence.
Frequently Asked Questions
What happens if someone moves backward through the stages of change in addiction?
Moving backward through the stages of change in addiction—sometimes called “recycling”—is common and not a sign of failure. People may return to earlier stages like contemplation or preparation after a setback, and this is a natural part of the process. In fact, research highlights that relapse and stage regression are expected, and each return can be an opportunity to learn new coping skills or adjust treatment approaches 14. By normalizing these setbacks, you help reduce shame and encourage individuals to re-engage with support. Every step, even backward ones, can foster growth and resilience if treated with understanding and compassion.
How long does it typically take to progress through each stage of change in addiction?
Progression through each stage of the cycle of change in addiction varies widely—there’s no set timeline. For some, moving from precontemplation to contemplation can take weeks or even months, especially if denial or ambivalence is strong. People who transition from one stage to the next within a month are twice as likely to take meaningful action within six months compared to those who remain stuck 4. The action stage often requires the most daily effort and may last several months, while maintenance is a lifelong process. Remember, everyone’s pace is different, and celebrating each milestone—no matter how small—helps sustain motivation and hope.
Can someone skip stages in the cycle of change in addiction?
Skipping stages in the cycle of change in addiction is rare, but people can sometimes appear to move quickly—especially during moments of crisis or external pressure. Most often, lasting change happens by progressing through each stage, even if some are brief or less visible. The Transtheoretical Model suggests that each stage builds essential motivation and skills for the next, so hurrying past a stage can increase the risk of setbacks or relapse. If someone seems to skip steps, it’s helpful to gently explore whether important groundwork—like building self-efficacy or resolving ambivalence—was truly addressed 4. Every step, no matter how small, matters for long-term recovery.
How can family members support someone through different stages of change in addiction?
Family members play a vital role in supporting someone through each stage of the cycle of change in addiction. In the precontemplation and contemplation phases, patience and nonjudgmental listening are your best tools—validate feelings and avoid pressuring for immediate change. As your loved one moves into preparation and action, practical help like attending appointments together or assisting with healthy routines can make a big difference. In maintenance, ongoing encouragement and celebrating small wins matter most. Research highlights that social support—including family involvement—significantly boosts motivation and helps people progress through the stages of recovery 8. Every gesture of understanding counts, even when the process feels slow.
What role does peer support play in moving through the stages of change in addiction?
Peer support plays a vital role throughout every stage of the cycle of change in addiction. Individuals with lived experience offer hope, break down isolation, and provide real-world strategies for overcoming obstacles. Whether someone is just starting to contemplate change or is working to maintain long-term progress, peer support makes the journey less lonely and more manageable. This approach is ideal for organizations aiming to boost motivation and build trust, especially when professional relationships alone aren’t enough. Research highlights that peer support can enhance engagement, foster self-efficacy, and help people stay connected during setbacks or relapse 8. Every shared story and moment of encouragement truly matters.
How do co-occurring mental health conditions affect progression through the stages of change in addiction?
Co-occurring mental health conditions—such as anxiety, depression, or PTSD—can make progression through the cycle of change in addiction more complicated. These conditions may increase ambivalence in the contemplation stage or add barriers to planning and taking action. For example, someone experiencing depression might struggle with motivation during preparation, while anxiety can heighten fear of change. This approach works best when treatment teams address both addiction and mental health needs together, using integrated care and flexible support options. Research shows that coordinated, stage-matched interventions improve engagement and outcomes for people with dual diagnoses 4. Every step forward, no matter how small, deserves recognition and support.
What are the chances of long-term success after reaching the maintenance stage of change in addiction?
After reaching the maintenance stage of the cycle of change in addiction, the outlook for long-term success grows more hopeful with each passing year. Research shows that 43% of people relapse within the first year of abstinence, but if someone maintains their progress for five years, the relapse rate drops dramatically to just 7% 4. This means the longer someone stays engaged in healthy routines and support, the greater their chances for ongoing recovery. Celebrate every milestone: even a single year in maintenance is a win. Remember, setbacks can happen, but continued support and self-compassion make long-term success possible for many.
Conclusion
Effective dual diagnosis treatment requires integrated approaches that address substance use disorders and co-occurring mental health conditions simultaneously. The evidence consistently demonstrates that treating these conditions in isolation produces suboptimal clinical outcomes, while comprehensive dual diagnosis treatment programs yield significantly higher rates of sustained recovery and functional improvement.
Structured dual diagnosis treatment through PHP and IOP modalities provides the therapeutic intensity necessary for meaningful progress while allowing clients to maintain essential life responsibilities. At Healing Rock Recovery in Billings, Montana, our dual diagnosis treatment programs integrate evidence-based modalities including CBT, DBT, and trauma therapy with medically assisted treatment protocols. Our approach incorporates both traditional evidence-based frameworks and culturally grounded interventions like the Wellbriety program, recognizing that effective dual diagnosis treatment must address the whole person within their cultural and spiritual context.
The availability of both in-person and virtual dual diagnosis treatment options expands access for professionals managing demanding schedules and for rural populations where specialized co-occurring disorder treatment remains limited. Our trauma-informed model acknowledges the high prevalence of adverse experiences underlying both substance use and mental health presentations, ensuring clinical interventions address root causes rather than symptoms alone.
As the field continues advancing our understanding of co-occurring disorders, integrated treatment models represent the clinical standard. Healing Rock Recovery’s Montana setting provides a therapeutic environment conducive to healing, while our flexible PHP and IOP structures support the practical realities professionals face during treatment. Effective dual diagnosis treatment creates the foundation for sustainable recovery outcomes and restored quality of life.
References
- StatPearls. Stages of Change Theory. https://www.ncbi.nlm.nih.gov/books/NBK556005/
- Enhancing Motivation for Change in Substance Use Disorder Treatment. https://library.samhsa.gov/sites/default/files/tip-35-pep19-02-01-003.pdf
- Relapse Prevention and the Five Rules of Recovery. https://pmc.ncbi.nlm.nih.gov/articles/PMC4553654/
- Stages of Change. https://tnchildren.org/wp-content/uploads/2014/11/Stages-of-Change.pdf
- Chapter 3—Motivational Interviewing as a Counseling Style. https://www.ncbi.nlm.nih.gov/books/NBK571068/
- Neuroscience: The Brain in Addiction and Recovery. https://www.niaaa.nih.gov/health-professionals-communities/core-resource-on-alcohol/neuroscience-brain-addiction-and-recovery
- Stages of Change Treatment Planner. https://www.dhs.wisconsin.gov/mh/conferences/stages-change-treatment-planner.pdf
- The Importance of Social Support in Recovery Populations. https://pmc.ncbi.nlm.nih.gov/articles/PMC10259869/
- Combining the Transtheoretical Stages of Change Model and the 12. https://pmc.ncbi.nlm.nih.gov/articles/PMC3520431/
- Wellbriety: 4 Laws of Change That Guide an Indigenous. https://recovery.com/resources/what-is-wellbriety/